- Basic information
- Management and staff
- Ambulance
- Center for the diagnosis and treatment of demyelinating diseases
- Center for Epilepsy (adult section)
- Cerebrovascular clinic
- Counseling for Parkinson's disease and other extrapyramidal disorders
- Cognitive impairment
- Center for the diagnosis and treatment of headaches
- Counseling for neurocutaneous diseases
- Dizziness Center
- Neuromuscular clinic
- Hereditary Ataxia Center - Adult section
- Inpatient department
- Video-EEG monitoring unit
- Laboratory complex
- Cerebrospinal fluid laboratory of the Institute of Immunology
- Examination of antineural antibodies
- EMG and EP laboratory
- EEG laboratory
- ENG laboratory
- Neurosonological laboratory
- History
- For the professional public
- Postgraduate teaching
- Thanks to our sponsors
- V-EEG monitoring - ordering
- Gallery
Welcome to the website of the Department of Neurology, Charles University, 2nd Faculty of Medicine and Motol University Hospital!
Our clinic develops the best traditions of the Czech and Slovak neurological schools. Using the latest neuroscience knowledge and medical technology, it provides comprehensive diagnostic, therapeutic and preventive care for patients with diseases of the nervous and myoskeletal system in cooperation with a number of clinical departments at the Motol University Hospital and the 2nd Medical Faculty of Charles University.
The clinic employs 41 physicians and PhD students, a speech therapist, 4 psychologists, a biochemist, specialized laboratory technicians and a team of nurses with a master's and bachelor's degree.
Continuity of patient care is ensured by good cooperation, especially with pediatric neurology, neurosurgery, spondylosurgery, oncology department, adult cardiocenter, imaging clinic, internal medicine and rehabilitation clinic of our teaching hospital.
Our clinic represents a teaching and clinical base for students of the 2nd Faculty of Medicine of Charles University and is an accredited workplace for postgraduate training of neurologists from all over the country.
prof. MUDr. Petr Marusic, Ph.D.
(224) 436 800
doc. MD Aleš Tomek, Ph.D., FESO
(224) 436 803
Hana Chvátalová
(224) 436 803
Clinic secretariat
224 436 801, 803
neurologie@fnmotol.cz
Reception ambulance
(224) 436 860
Management and staff
Head:
prof. MD Petr Marusič, Ph.D., phone: 224 436 800
Medical representative, primary:
doc. MD Aleš Tomek, Ph.D., FESO, phone: 224 436 803
Teaching representative:
MD David Krýsl, Ph.D., phone number 224 436 804
Science and Research Representative:
prof. MD Jakub Hort, Ph.D., phone number 224 436 879
Head nurse:
Hana Chvátalová, phone: 224 436 803
Secretariat
Sanitary
Bc. Gabriela Křížková, phone: 224 436 802
Educational
Bc. Romana Lipinová, tel. 224 436 800
Science and research
Vladislava Fulínová, tel. 224 436 809
e-mail of the clinic: neurologie@fnmotol.cz
Clinic doctors
MD Amlerová Jana, Ph.D.
MD Daniel Baumgartner
MD Bednářová Martina (including maternity leave)
MD Benešová Kateřina
MD Blichová Zuzana
prof. MD Bojar Martin, CSc.
MD Buchtelíková Markéta
MUDr. Cerman Jiri, Ph.D.
as. MUDr. Black Rudolf, CSc.
MD Drasnarová Hana
MD Elišák Martin, Ph.D.
MD Fábera Petr, Ph.D.
MD Hadzic Haris
MD Hana Halmová, Ph.D.
MD Havlicek Martin
as. MD Aleš Homola, Ph.D.
MD Janský Petr
doc. MUDr. Jerabek Jaroslav, CSc.
MUDr. Kadlecova Alexandra, Ph.D.
MD Kajšová Michaela
MD Simona Karamazov
MD Petra Kešnerová, Ph.D.
MD Kinštová Lenka
MD Jana Kluhova
MD Kmetony Silvia
MD Kritová Hana
MUDr. Krysl David, Ph.D.
MD Kuzmiak Michaela, Ph.D.
prof. MD Laczó Jan, Ph.D.
MD Laczó Martina, Ph.D.
MD Lachmann Hynek
MD Lerch Ondřej, Ph.D.
MUDr. Mgr. Libertinova Jana, Ph.D.
MUDr. Magerova Hana, Ph.D.
MD Martinkovic Lukáš
MD Karolina Marton
MUDr. Matousova Zuzana
as. MD Radim Mazanec, Ph.D.
MD Mencl Michael
MD Mensová Lívie (including maternity leave)
MD Mojžišová Hana
MD Zuzana Nedelská, M.Sc., Ph.D.
MD Sunday Tomas
MD Mute Eve, Ph.D. (including maternity leave)
MD Nováková Martínková Julie
MD Viktoria Ogurčáková
MD Olšerová Anna
MUDr. Paulas Schwabova Jaroslava, Ph.D.,
MD Petržalka Marko, Ph.D.
MD Veronika Potočková, Ph.D.
MUDr. Kryšil Kryštof
MUDr. Rockova Petra, Ph.D.
MD Sečník Juraj, Ph.D.
MD Saint Clare
MD Šarbochová Ivana
MD Skorvagova Adéla
MD Šrámek Martin
MD Šrámková Tereza (item no. maternity leave)
MD Šulc Vlastimil
MD Trubačik Mokrišová Ivana, Ph.D. (including maternity leave)
MD Tuček Borek
doc. MUDr. Vyhnálek Martin, Ph.D.
MD Wolfová Ivana (including maternity leave)
as. MD Zárubová Jana
as. MD Zarubová Kateřina
MD Game Michaela
Neurological clinic
Chief physician:
doc. MD Martin Vyhnálek, Ph.D., tel. 224 436 860
Deputy Chief Physician:
MUDr. Zuzana Matoušová, phone 224 436 860
Ambulance doctors:
prof. MD Jan Laczó, Ph.D.
MD Tomáš Nedělka, Ph.D.
Station nurse:
Martina Bušová, tel. 224 436 860
Ambulance operation
Within the outpatient department of the Department of Neurology, patients are treated in the acute admission clinic, which is located on the premises of the Department of Adult Emergency Reception (floor -P, reception in the middle of the hall) and in specialized counseling centers located on the 2nd floor, node D.
Reception ambulance
The neurological outpatient clinic provides treatment to patients with acute nervous system disorders sent by a general practitioner or district neurologist, or by the adult emergency department. The main task is to determine the basic diagnosis and decide whether hospitalization in a neurological bed is necessary.
If your medical condition requires it, you will be examined by a neurologist on the same day and you will then be recommended follow-up hospital or outpatient care.
Due to operational and capacity possibilities, we recommend it in non-acute cases, seek an examination at the nearest neurological clinic in the place of residence. If in doubt, please consult your GP.
If you suffer from an illness that requires repeated neurological examinations/checkups, please seek the care of one of the outpatient neurologists outside of our hospital. Due to capacity reasons, long-term follow-up of patients at our clinic's outpatient clinic is unfortunately not possible.
Office hours: Monday to Friday 8:00 - 16:00
For urgent cases, the admission clinic is open on weekdays until 19:00 (the last patient is admitted for examination at 18:30).
Sudden, health or life-threatening conditions (eg suspected stroke) are treated continuously at the Adult Emergency Reception Department (floor -P) with permanent availability of a neurological counselor.
Specialized centers and counseling centers
The following counseling centers and centers have been set up within the clinic. See the following links for details:
- Center for the diagnosis and treatment of demyelinating diseases
- Center for Epilepsy (adult section)
- Cerebrovascular clinic
- Counseling for Parkinson's disease and other extrapyramidal disorders
- Cognitive impairment
- Center for the diagnosis and treatment of headaches
- Counseling for neurocutaneous diseases
- Advice for dizzy states
- Neuromuscular clinic
Procedure for ordering a superconciliary examination:
If you are already being treated for a neurological disease and your doctor requires an expert assessment from our clinic (second opinion), we need to provide the relevant documentation in advance - see below.
Requests for outpatient outpatient examinations should be sent in writing to:
Department of Neurology, 2nd Faculty of Medicine, Charles University and Motol University Hospital - ambulance
V Úvalu 84
150 06 Prague 5
Or by e-mail: neurologickaambulance@fnmotol.cz
Please attach to the application:
- summary and request for an examination from your doctor
- copies of examinations performed so far, event. reports from previous hospitalizations
- Your address + telephone contact/e-mail.
Based on the documents you send, we will select the most suitable doctor and inform you of the date of the examination. In justified cases, we will invite you to hospitalization.
For examination (or hospitalization), request previously performed imaging examinations (CT or magnetic resonance imaging) on CD. An alternative is to send it electronically via ePACS, which can be arranged by your doctor.
Your doctor can also contact the doctors of our clinics directly and arrange an examination with them.
Center for the diagnosis and treatment of demyelinating diseases
Head of the center:
MUDr. Mgr. Jana Libertinova, Ph.D.
Doctors:
MUDr. Petra Rockova, Ph.D. (Mon - Wed)
MUDr. Martin Elišák, Ph.D. (Wed - Fri)
MD Hana Mojžišová
MD Marko Petržalka
MD Klára Svátová
Sisters:
Jana Jindrová
Lenka Ondračková
Michaela Kosakova
(all nurses specialize in working in the MS center)
Secretariat:
Monika Moravcová
Medical consultations for existing patients Monday - Friday from 13:00 - 14:00 on the phone 224 436 881
For the first examination, patients can order by e-mail at the address mscentrum@fnmotol.cz, please include contact details including address in the e-mail.
The Center for the Treatment and Diagnosis of Demyelinating Diseases started its activities in 2000. Currently, more than 2000 patients, mainly with multiple sclerosis (MS), are monitored and treated here. Patients come to the center with a diagnosis that has already been established, or it is specified differentially during hospitalization at the Neurological Clinic. In addition to adult patients, we also provide follow-up care for patients of the Department of Pediatric Neurology at Motol FN.
All patients are treated with first- or second-line drugs, provided the indication criteria are met. Some patients are being offered new drugs as part of ongoing clinical trials. Patients treated with interferons-β are monitored for treatment by detecting the production of neutralizing antibodies and examining MxA protein mRNA.
The center includes a day hospital, where intravenous treatment is administered or therapy requiring a monitored bed is initiated.
Patient care within the center is comprehensive, we work closely with other departments of the Motol University Hospital:
- Department of Urology - treatment of sphincter disorders, urodynamic examination (Michal Rejchrt, MD, Klára Havlová, MD)
- Department of Ophthalmology - examination and monitoring of patients with optic neuritis, OCT examination (MUDr. Květoslava Ferrová)
- Clinic of rehabilitation and physical education medicine - circuit training specially designed for patients with MS, individual outpatient rehabilitation programs, inpatient rehabilitation stays (principal Martina Kövári, M.D.)
We also solve specific patient problems in cooperation with clinical psychologists (PhDr. Martin Jung, Department of Neurology, University Hospital Motol, PhDr. Eva Růžičková, www.psychologickapece.cz)
We monitor pregnant patients during pregnancy and in the sixth trimester in cooperation with gynecologists (Petra Hanulíková, MD, ÚPMD)
The center is involved in research activities - monitoring the effectiveness of biological treatment, predicting disease activity, the issue of cognitive dysfunctions, the center's doctors are authors/co-authors of a number of review articles and chapters in professional literature.
Motol Epilepsy Center is a specialized workplace that provides comprehensive diagnostic, medical and nursing care for the entire spectrum of pediatric and adult patients with epilepsy.
The center is based on close cooperation Pediatric neurology clinics a Departments of Neurology, 2nd Medical Faculty, Charles University and University Hospital Motol. Patients are examined and treated in the relevant clinics, complicated cases (especially patients with refractory epilepsy) are discussed at joint seminars within the activities of the center. The diagnostic and treatment procedures used in both parts of the center meet all internationally recognized criteria.
Counseling for seizure disorders (outpatient part of the center)
phone: (702) 001 925
Email: epilepsie@fnmotol.cz
Doctors
prof. MUDr. Petr Marusic, Ph.D. - office hours (after ordering) - Monday 13:00 -17: 00, Thursday 9: 00-13: 00
MD Jana Amlerová, Ph.D. - office hours - individually by appointment
MD Martin Elišák, Ph.D. - office hours (after ordering) - Tuesday
MD Hana Krijtová - office hours (after ordering) - Tuesday 9:00 -13: 00, Wednesday 9:00 - 13:00
MD Jana Zárubová - office hours (after ordering) - Tuesday, Friday
MD Vlastimil Šulc
MD David Krysl, Ph.D.
MD Adam Kalina
MD Peter Faber
MD Jana Kluhová
- Request for antibody testing (216,92 KB)
The cerebrovascular clinic provides care for patients after a stroke (CMP) in connection with hospitalization in the neurological ICU, and the standard ward determines the optimal secondary prevention of CMP. We also offer superconsulting care for primary and secondary prevention for particularly at-risk patients from all over the country.
Ordering patients (including neurosonological examination) tel. 224 436 874, Monday to Friday, 11 am - 12 noon,
or email address cmp@fnmotol.cz
Doctors clinic
doc. MD Aleš Tomek, Ph.D., FESO
MD Ivana Šarbochová
MD Hana Magerová, Ph.D.
MD Jaroslava Paulasová Schwabová, Ph.D.
MD Martin Sramek
MD Petr Janský
MD Anna Olšerová
MD Silvia Kmetonyová
nurse of cerebrovascular clinic: Tereza Valentová Šípová
The specificity of the clinic is the effort for individualized secondary prevention of stroke, especially the solution of issues related to individual response to antithrombotic drugs (reducing blood clotting). The goal is to determine the most detailed and correct secondary prevention after CMP, because stroke recurrence has twice the mortality rate of the first stroke!
The counseling center focuses on patients with CMP mainly on:
1) The issue of determining the cause of CMP at a younger age - in patients who experience CMP under the age of 50, the classic and well-known risk factors for atherosclerosis (such as hypertension, obesity, diabetes, smoking, etc.) may not be the cause. It can be one of the many dozens of rare causes of CMP, such as congenital diseases (CADASIL, Fabry) or inflammatory arterial lesions (vasculitis) and many others that require a very thorough examination program. If we find the cause, we can offer targeted preventive treatment.
2) Pharmacogenetics of warfarin - analysis of VKORC1 and CYP2C9 genes, which determine the size of the necessary and optimal dose of warfarin. Advice for patients with atypically low required warfarin dose (below 2 mg per day) or with repeated "intoxications" during warfarin treatment
3) Indications for invasive preventive procedures after CMP - we indicate patients to procedures that can prevent further recurrence of CMP, such as closure of the foramen ovale patens, carotid endarterectomy or stenting, bypass between the internal and external carotid arteries
4) Issues related to "resistance" to antiplatelet drugs (k. acetylsalicylic, clopidogrel, ticlopidine, dipyridamole) - in cooperation with DNA laboratory NNH, Department of Clinical Hematology FN Motol as Department of Clinical Biochemistry, Hematology and Immunology Na Homolce Hospital we investigate laboratory resistance to the following drugs: optical aggregometry, impedance aggregometry CYP 2C19.
Doctors clinic
As. MD Kateřina Zárubová, head of the counseling center
- order tel. 224 436 860 or 224 436 885
MUDr. Zuzana Matousova
- order tel. 224 436 860
doc. MD Martin Vyhnálek, Ph.D.
- office hours Thursday 8: 30-15: 30, Friday 10-14, order 224 436 860
The content of care in our counseling center
The clinic provides diagnostic and therapeutic services to patients with Parkinson's disease, Parkinson's syndromes, tremor and other extrapyramidal disorders, such as chorea, dystonia, myoclonus and other abnormal movements.
The prognosis of extrapyramidal diseases has changed fundamentally in recent years with the possibilities of modern pharmacotherapy, surgical treatment and other procedures.
The counseling center uses the possibilities of complex diagnostic equipment of the teaching hospital (laboratory, electrophysiological, CT, MRI, SPECT, DaTSCAN imaging examinations). Standard and above-standard neurological beds are available within the neurological clinic.
It offers the possibility of using new therapeutic procedures in the treatment of Parkinson's disease with the provision of state-of-the-art drugs. It enables the indication of neurosurgical procedures (implantation of brain stimulators). The rehabilitation program is also a part of the comprehensive treatment.
In cooperation with the Rehabilitation Clinic, it offers the possibility of using a specially focused rehabilitation program for patients with Parkinson's disease.
It will provide those interested with detailed information about Parkinson's disease, and will provide contact with Parkinson's (a self-help organization that associates patients with this disease).
Cognitive center
Doctors clinic:
prof. MD Jakub Hort, Ph.D., head of the center
doc. MD Martin Vyhnálek, Ph.D.
prof. MD Jan Laczó, Ph.D.
Counseling coordinator:
Vladislava Fulínová
ordering checks - e-mail: vladislava.fulinova@fnmotol.cz phone: 224 436 809
see ordering new patients below
The following also participate in the activities of the counseling center:
MD Jiří Cerman, Ph.D.
MD Ondrej Lerch
MD Martina Laczó
MD Zuzana Nedelská
Psychologists:
Mgr. Tomas Nikolai, Ph.D.
M.Sc. Hana Horáková, Ph.D.
M.Sc. Adéla Mazancová
M.Sc. Katerina Čechová
M.Sc. Veronika Matusková
ORDERING NEW PATIENTS
Due to capacity reasons, we are forced to almost stop examining new patients, and we are currently examining and accepting for follow-up almost exclusively patients whose health condition requires monitoring and treatment at the faculty workplace. These are mainly patients in the early stage of cognitive deficits or patients with unclear or rare diagnoses who are referred to us by their attending neurologists. A large proportion of patients with suspected cognitive impairment are t.č. For the reasons mentioned above, she is being monitored by our colleagues outside the hospital - outpatient neurologists and psychiatrists with whom we work and who turn to us for further consultations. If your doctor thinks that the examination options at your place of residence have been exhausted and you need an expert examination at our workplace, this is generally possible in the so-called superconciliary examination regime.
Requests for outpatient outpatient examinations should be sent in writing to:
Mrs. Vladislava Fulínová
Department of Neurology, 2nd Medical Faculty, Charles University and University Hospital Motol
V Úvalu 84
150 06 Prague 5
Or by e-mail: vladislava.fulinova@fnmotol.cz
Please attach to the application:
- summary and request for an examination from your doctor
- copies of examinations performed so far, event. reports from previous hospitalizations
- Your address + telephone contact/e-mail.
For an examination (or hospitalization), request previously performed imaging examinations (CT or magnetic resonance imaging) on a CD. An alternative is to send it electronically via ePACS, which can be arranged by your doctor.
Your doctor can also contact the doctors of our clinics directly and arrange an examination with them.
CENTER FOCUS
The issue of cognitive neurology cannot be limited to the issue of Alzheimer's disease, although this disease is the most common cause of cognitive impairment (memory, speech, practical, gnostic, executive functions). Alzheimer's disease should be called Alzheimer's-Fischer disease, because at the same time that Alois Alzheimer described a single patient, a Czech native from Slaný prof. Oscar Fischer described a total of 12 cases. Thanks to his unfavorable fate and death during the occupation and the irony of fate, this important Czech primacy was forgotten for many years. Our counseling center would like to continue the tradition of predecessors of European significance, such as Oscar Fischer or Arnold Pick, who described frontotemporal dementia. Due to its clinical and scientific results, as well as its staff, the counseling center is one of the leading European workplaces dealing with the diagnosis of patients with cognitive disorders. It offers modern diagnostic and treatment procedures that have been developed in collaboration with foreign institutions (Mayo Clinic, Rochester, USA, University of South Florida, Tampa, USA, Massachusetts General Hospital, Boston, USA, Montpelier, France, Queensland Brain Institute, Australia) . These are mainly modern screening protocols for patients over the age of 50 with subjective cognitive decline (SCD), patients with mild cognitive impairment (MCI) and various types of dementia. The main focus is on the prediction, diagnosis and treatment of Alzheimer's disease, Lewy body dementia, frontotemporal dementia, Parkinson's plus syndromes, and many other rare causes of cognitive deficits. To a limited extent, the counseling center also operates in the field of diagnosis and treatment of diseases causing cognition disorders at a younger age - eg intoxication, post-traumatic conditions, conditions after vascular and inflammatory diseases of the brain. The center does not deal with the diagnosis or treatment of primarily psychiatric diseases leading to cognitive impairments.
The center uses the possibilities of comprehensive diagnostic equipment of the teaching hospital and partner workplaces (laboratory, CT, MRI, SPECT, DaTSCAN, amyloid PET, examination of biomarkers in cerebrospinal fluid, genetic examination). Within the neurological clinic, standard and above-standard neurological beds are available for short diagnostic stays. However, these beds are not intended for long-term hospitalization or follow-up social care for patients with cognitive deficits.
The center closely links clinical and research activities. It is the application of the latest research findings in diagnostic processes that enables earlier detection of diseases such as Alzheimer's disease or other neurodegenerative diseases. Within the center, it is possible in some cases to perform a completely unique neuropsychological examination and examination of spatial memory, which is affected very early. The special Amun facility, which is owned by the Department of Neurology and whose previous version was developed in cooperation with the Academy of Sciences of the Czech Republic, is used for this purpose. Some special neuropsychological tests were invented and published for the first time at our workplace. In addition to routine examinations, the center also offers advanced MRI signal processing options - DTI techniques, volumetry and more. Some biochemical examinations, which are not routinely available in the Czech Republic, are also carried out thanks to the centre's integration into European projects and grant programs.
Fig .: device for examination of spatial cognition - Amun
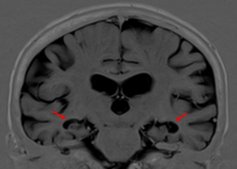
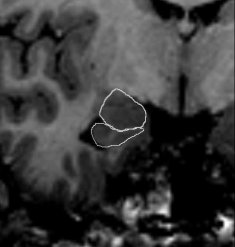
Giant. MRI examination of hippocampal atrophy
The center offers the possibility of using new therapeutic procedures in the treatment of Alzheimer's disease and other neurodegenerative diseases with the provision of state-of-the-art drugs. The clinic is conducting clinical trials with new drugs that are not yet commonly available, but may help in the treatment of as yet incurable diseases. An example is a program with beta-secretase inhibitors or passive and active immunization against beta-amyloid and tau protein. Part of the comprehensive treatment is the possibility of directing patients to social counseling and cognitive training in cooperation with other workplaces.
The center also offers the possibility of directing to counseling services or contact points of the Czech Alzheimer's Society, which can advise on social and legal issues.
The Center for Diagnosis and Therapy of Headaches focuses mainly on the diagnosis and treatment of patients with headaches who have not been able to sufficiently influence their problems during treatment in catchment neurological workplaces. The center has a supra-regional scope and provides superconsulting services. In severe cases, it is possible to take the patient into further care.
We focus on patients with complicated migraine and cluster headache, patients with multiple types of headaches and patients with analgesic overuse (medication overuse headache).
The center has a complete diagnostic complement within the neurological clinic (cerebrospinal fluid, electrophysiological and neurosonological examinations) or within the Motol University Hospital (MRI, CT). We cooperate with specialists in the field of psychology, psychosomatics, algesiology, medical rehabilitation and neurosurgery.
In indicated cases, we offer patients infusion therapy during hospitalization, application of botulinum toxin A or administration of monoclonal antibodies against CGRP as part of prophylactic therapy for migraine.
The condition of the examination in our center is a medical report from the attending neurologist.
Chief physician of the center: MUDr. Zuzana Matousova
Contact and order:
tel. 702 001 909 - in the form of an SMS message
Based on e-mail or SMS, we contact patients with the date of the examination.
Counseling for neurocutaneous diseases
Doctors clinic:
MD Lenka Kinštová, head of the counseling center
order tel: 702 001 872
office hours Tuesday 13:00 - 16:00
The content of care in our counseling center
The clinic provides diagnostic and therapeutic services to patients with neurocutaneous syndromes.
Neurocutaneous syndromes are genetically determined systemic diseases most often affecting the nervous system, skin and eye with a tendency to tumor growth. The most well-known clinical units include neurofibromatosis, tuberous sclerosis, and vascular syndromes - Sturge-Weber syndrome, Ataxia telangiectasia, Von Hippel-Lindau disease.
The counseling center uses the possibilities of diagnostic equipment of the teaching hospital (laboratory, electrophysiological, CT, MRI, genetic diagnostics) and other medical facilities (LGK, PET). Interdisciplinary cooperation with the ophthalmic, dermatological, rehabilitation, oncological, orthopedic, spondylous and neurosurgical teams enables comprehensive therapeutic and diagnostic care. Within the neurological clinic, neurological beds and the use of a video-eeg monitoring unit are available.
The counseling center takes over patients with these genetic syndromes from the FNM children's specialist counseling center with the same focus, thus guaranteeing the continuity of care for these patients and their equally ill relatives within one medical facility.
Logo Vestibular clinics today are reminiscent of the often neglected link between medicine and other natural science disciplines. Vertigo is not only a technical term, but also, for example, a genus of snails from the lung subclass. This small creature also occurs in the Czech Republic.
We thank our leading malacologist RNDr. Vojena Ložek, Csc.
Doctors clinic
Doc. MUDr. Jaroslav Jerabek, CSc.
As. MUDr. Rudolf Cerny, CSc.
The vestibular clinic and laboratory of the Department of Neurology is part of the comprehensive Neuro-Otology Center of Charles University in Prague, 1st and 2nd Medical Faculty and the University Hospital in Motol (Center), which includes the Department of Neurology, ENT and Rehabilitation Clinic. Our workplace is thus able to provide detailed diagnostics of vestibular and tribal disorders of various origins, including specialized examinations of several (various, necessary…) medical disciplines. Follow-up medical care is a comprehensive program including pharmacotherapy, ENT treatment and individualized rehabilitation program, incl. the possibility of using biological feedback methods.
The center provides a comprehensive diagnostic service for patients with balance disorders, oculomotor disorders and focal lesions in the brainstem area. The working team of the laboratory provides clinical and objective functional, electrophysiological diagnostics and treatment in this area. In the laboratory, we examine an average of 350 to 400 patients a year. The catchment area consists mainly of Prague 5, 6 and their wider surroundings. However, requests for super-counseling consultation come from all over the country.
LABORATORY EQUIPMENT
The laboratory equipment enables objective and quantitative diagnostics of the labyrinth function by means of a series of rotary tests, caloric examination by the bithermal method and by air (in cases of tympanic pathology). Objective evaluation of central vestibular syndromes and oculomotor disorders are enabled by visually provoked eye movements - optokinetic nystagmus, tracking eye movements, saccadic eye movements. All techniques are evaluated quantitatively by computer analysis of an electronystagmographic record online.
In addition to electronystagmography (ENG, Toennies PRO system ®) we have a video-oculographic registration of eye movements -VOG. This is a very sensitive non-contact eye movement technique that eliminates electrical artifacts that complicate the evaluation of ENG eye movement records.
The posturographic laboratory is equipped with the Synapsis ® stabilometric system enabling registration of static and dynamic stabilometry (recording of body center of gravity movements) and training in maintaining the correct body position within balance training using the biological feedback method.
Disorders of vertical stabilization of standing and walking can also be assessed by optical recording - Cranio-corphography.
We use VOG, quantitative evaluation of subjective vertical and Maddox glasses to evaluate eye torsion.
The vestibular laboratory also has a universal electrophysiological device Synergy ® equipped for recording of stem auditory evoked potentials, blink reflex and examination of vestibular myogenic evoked potentials (VEMP), which represent the current standard of objective examination of otolith function.
If necessary, a complete ENT and audiological examination is available within the Center.
CONSULTANCY ORDER
Appointments to the consulting room and laboratory examination (ENG, stabilometry, video-oculography, VEMP) are provided by the assistant on the telephone number 602 277 121, Wednesday and Thursday between 10:00 a.m. and 12:00 p.m., and at the address neuro.otologie@fnmotol.cz
It is necessary to recommend a specialist, as this is a specialized, so-called superconsiliary examination.
Contact a doctor for an examination in the clinic:
As. MUDr. Rudolf Cerny, CSc.
Doc. MUDr. Jaroslav Jerabek, Csc.
jaroslav.jerabek@lfmotol.cuni.cz
MD Michaela Kuzmiak
MD Lukáš Martinkovič
TEACHING
In the undergraduate clinical neurology courses (compulsory and optional courses), we introduce fifth-year students of the faculty to the basics of clinical and laboratory assessment of balance disorders - one-hour internship and seminar. We regularly organize postgraduate courses in neurotology for those interested from among the professional public.
We also welcome all those interested in an individual internship in this area, the program proposal is given according to the attached syllabus, which is always individually adapted to the requirements of those interested.
Contact the trainer:
ASr. MUDr. Rudolf Černý, CSc.
doc. MUDr. Jaroslav Jerabek, CSc.
jaroslav.jerabek@lfmotol.cuni.cz
Information can also be obtained at the training department of the Motol University Hospital. We offer students the possibility of student scientific professional activities at our workplace, which is equipped with modern electrophysiological and data analysis facilities, including computer technology, statistical and analytical software. We can also offer a demonstrator position to serious applicants.
The clinic provides diagnostic and therapeutic counseling for patients suffering from motor neuron diseases, peripheral and autonomic neuropathies, neuromuscular disorders, skeletal muscle diseases and neuropathic pain. The counseling center provides consulting services to outpatients and hospitalized patients at the Motol University Hospital and works closely with the Department of Pediatric Neurology at the Motol University Hospital in providing health care to patients and adults.
The neuromuscular diseases program includes, in addition to the provision of health care, extensive scientific and experimental research, which goes beyond the Prague region and has not only a national but also an international dimension.
Staffing and telephone contact:
As. MD Radim Mazanec, Ph.D. - head of the neuromuscular program
order by e-mail: andrea.srbova@fnmotol.cz or tel .: (720) 816 883
MD Hynek Lachmann - electromyography and evoked potentials
MUDr. Borek Tucek - electromyography
MD Tomas Nedelka - diagnosis of disorders of the autonomic nervous system
MD Veronika Potočková - electromyography + diagnostics of autonomic nervous system disorders
MD Daniel Baumgartner - diseases of motor neurons and myasthenia gravis
Alena Zdráhalová – station nurse and head laboratory technician of electromyography and evoked potentials
phone: 224 436 867
Andrea Srbova, sister
Radka Maierová, sister
Coordinator
phone: 224 436 817
Monday-Friday 14:00-15:00
use the e-mail address for communication: nmc.fnm@gmail.com
The main areas of consulting activities of the counseling center
1. Diseases of motoneurons
Motor neurone disease includes two basic groups of patients:
a / genetic disorders - spinal muscular atrophy (SMA) and bulbospinal muscular atrophy (BSMA), so-called Kennedy disease
b / neurodegenerative disorders - amyotrophic lateral sclerosis and its variants
2. Peripheral neuropathy
Peripheral neuropathies represent a wide range of peripheral nerve disorders that have different causes (genetic, metabolic, inflammatory, toxic, etc.), different clinical symptoms, and different treatments. The largest group of patients are patients with endocrine neuropathies (diabetes mellitus, thyroid disease), inflammatory neuropathies (chronic inflammatory demyelinating neuropathy CIDP, acute inflammatory neuropathy - Guillain's Barré syndrome, neuroborreliosis), toxic neuropathies (after cancer treatment and other drugs) conditioned (hereditary) neuropathies.
The diagnostic algorithm includes neurological and electromyographic examinations, blood tests. In frequent cases, lumbar puncture and cerebrospinal fluid examination are necessary. Only in some cases is it necessary to perform a nerve biopsy of the peripheral nerve (most often n.suralis). About 20% of patients fail to detect the cause of peripheral neuropathy (so-called idiopathic neuropathy) even after a detailed examination, including a nerve biopsy.
Causal treatment is only possible if the exact cause of peripheral neuropathy is determined. If the cause is unknown, some unpleasant symptoms of neuropathy (neuropathic pain) may be affected or supportive care may be provided (usually B vitamins, rheology, phytotherapeutics).
3. Disorders of neuromuscular transmission
Diseases caused by a neuromuscular transmission disorder are most often myasthenia gravis and myasthenic syndrome. It is an autoimmune disease of the neuromuscular disc, which is manifested by various symptoms of fluctuating muscle weakness. The condition may be manifested by eye symptoms (decreased eyelids, double vision), disorders of articulation and swallowing, or weakness of the skeletal muscles of the torso and limbs. Correct and timely diagnosis will allow effective treatment to be initiated, which leads to stabilization of the condition. The diagnosis is made in collaboration with immunologists, radiologists and neurophysiologists. After diagnosis, further treatment is consulted with the Center for Myasthenia Gravis at the Department of Neurology, First Faculty of Medicine, Charles University and General Hospital.
4. Skeletal muscle diseases - myopathy
Myopathies, or primary skeletal muscle disorders, represent a very diverse and broad group of diseases. They include both genetically determined (hereditary) myopathies and acquired myopathies (eg inflammatory, metabolic, toxic). The causes of myopathies are very varied and a number of tests are needed to detect them. Some are commonly available (creatine kinase and myoglobin biochemistry or needle electromyography), others are less common (DNA analysis, muscle biopsy). In addition to skeletal muscle examination, examination of the heart (ECG, echocardiography) and respiratory functions (spirometry, X-ray of the heart and lungs) is always necessary.
In addition to general diagnostic activities, the counseling center focuses primarily on monitoring patients with muscular dystrophies and congenital myopathies. Within the Motol University Hospital, he cooperates with the Institute of Pathological Anatomy on histological diagnostics of muscle diseases and with the Institute of Biology and Medical Genetics on molecular genetic diagnostics of muscle diseases.
Medical care uses the wide possibilities of the Motol University Hospital (cardiology, spirometry, eye examinations, rehabilitation, orthopedics). The cooperation with the Department of Pediatric Neurology is very close to maintaining the continuity of health care for patients in adulthood.
5. Hereditary neuropathy - Charcot-Marie-Tooth disease
Health care for patients with hereditary neuropathies is one of the basic programs of national importance. The counseling center provides the function of a national center for these patients with CMT disease. The department coordinates consulting activities, which include a diagnostic part (neurological examination + electromyography + targeted indication for genetic tests) and a therapeutic part (interdisciplinary cooperation with geneticists, orthopedists, prosthetics and rehabilitation workers). Within the FNM there is a very close cooperation with the Department of Pediatric Neurology and DNA Laboratories of the ÚBLG, in the treatment part with the Rehabilitation Clinic of the FNM and the 2nd Orthopedic Clinic of the FNM.
6. Autonomic neuropathy
A very important part of the neuromuscular program is research, diagnosis and treatment of disorders of the autonomic nervous system. These disorders are accompanied mainly by diabetes mellitus, inflammatory, toxic and some genetic disorders. Laboratory diagnostics is provided in cooperation with the Institute of Neurosciences, 2nd Faculty of Medicine, Charles University and FNM. Treatments require comprehensive and interdisciplinary collaboration, especially with cardiologists, urologists and diabetologists.
7. Neuropathic pain
The counseling center provides consulting services for patients suffering from neuropathic pain. These are most often conditions of painful diabetic neuropathy, lumbar spine pain with radicular syndromes, postherpetic neuralgia or post-traumatic neuropathic pain. For complex and resistant forms of neuropathic pain, the clinic provides more complex neuromodulatory treatment procedures in cooperation with the Center for the Study and Treatment of Pain at the Motol University Hospital.
Hereditary Ataxia Center - Adult section


Center manager:
doc. MD Martin Vyhnálek, Ph.D.
Neurologists - adult part:
MD Jaroslava Paulasová-Schwabová, Ph.D.
MD Michaela Kuzmiak
doc. MUDr. Jaroslav Jerabek, CSc.
MD Simona Karamazova
Clinical geneticist: MUDr. Emilie Vyhnalkova, Ph.D.
Laboratory geneticist: Mgr. Zuzana Musova, Ph.D.
Physiotherapist: doc. PaeDr. Ondřej Čakrt, Ph.D.
Focus and characteristics of the workplace
The Motol University Center for Hereditary Ataxia deals with comprehensive diagnosis and care of patients with inherited ataxias - rare causes of balance and coordination disorders, including spinocerebellar ataxia (SCA), Friedreich's ataxia, metabolic and mitochondrial ataxia and other rare diseases. Within the center, we also take care of patients with hereditary spastic paraparesis.
The center is a member of the European Reference Network for Rare Neurological Diseases (ERN-RND) and a reference center for pediatric and adult patients with ataxias from all over the Czech Republic.
Within the Motol University Hospital, the center has comprehensive diagnostic tools at its disposal, including stabilometry, electronystagmography, examination of evoked potentials, laboratory and imaging methods. The application of advanced genetic methods of next generation sequencing (NGS) in close cooperation with the Institute of Biology and Medical Genetics enables the identification of very rare forms of ataxia and the clarification of long unresolved cases.
The center, in cooperation with foreign scientific teams, is involved in research activities in the field of diagnostics and monitoring of atactic diseases and the development of new treatments (pharmacological, including biological or gene therapy, or non-pharmacological, eg physiotherapeutic or occupational therapy procedures).
Instructions for ordering a superconciliary examination
The Center for Hereditary Ataxias offers the possibility of superconsulting examinations for patients from all over the Czech Republic and, after approval by the insurance company, also from Slovakia, based on the recommendation of their attending neurologist.
If you are in the care of a patient with chronic cerebellar ataxia, whom you wish to send to the center, please perform basic examinations to exclude acquired forms of ataxia - ie detailed anamnesis including three-generation pedigree, clinical examination, basic laboratory tests and MRI. , event. spinal cord. More detailed information for doctors is available here:
https://www.neurologiepropraxi.cz/pdfs/neu/2019/05/05.pdf
Ordering to the center is possible by e-mail at ataxie@fnmotol.cz.
Please attach copies of previous examinations or reports from previous hospitalizations and send MR images via ePACS.
Location
The adult part of the center is located in the outpatient department of the Neurological Clinic of the Motol University Hospital, on the 2nd floor at node D.
ICU - Stroke Center accredited by the Ministry of Health of the Czech Republic
Chief Physician of the Motol University Hospital Center: doc. MUDr. Ales Tomek, Ph.D. FESO, by phone: 224 436 803
Chief ICU: MD Ivana Šarbochová, phone number 224 436 853
Station nurse: M.Sc. Tereza Koláčná, phone 224 436 807, sister by phone: 224 436 836
The unit has 12 beds and mainly provides care for patients with strokes.
I. inpatient station and video-EEG monitoring unit
Chief physician: MD Michaela Kuzmiak, Ph.D., tel. 224 436 830, 865
Video-EEG monitoring unit: MD David Krysl
Station nurse: Bc. Lucia Simáčková, phone 224 436 806, sister by phone: 224 436 830
The first station has 21 standard beds and 3 beds of the video-EEG monitoring unit.
II. bed station
Chief physician: MD Lenka Kinštová, tel. 224 436 831, 858
Station nurse: Radka Paterová, phone 224 436 808, sister by phone: 224 436 831
II. the station has 27 standard beds and 3 beds with above-standard room equipment.
Video-EEG monitoring is an examination method in which EEG (electrical activity of the brain) and video (clinical manifestations of the patient) are recorded synchronously. Hospitalization usually lasts 5-7 days.
The examination is performed on the basis of recommendation of the attending physician (usually a neurologist)
Ordering for video-EEG monitoring
It is possible to order a patient for the examination email (epilepsie@fnmotol.cz), possibly in writing.
The doctor indicating the examination sends to the above e-mail (or to the address of the center) request for video-EEG monitoring with detailed report about the patient and the formulated question that this examination is supposed to solve. A prerequisite for performing a video-EEG is the presence of seizures with such a frequency that it is likely to be captured during the examination. The main indications for video-EEG monitoring include:
- Differential diagnosis of epileptic and non-epileptic seizures
- Determination of the type of epileptic seizures
- Drug-resistant epilepsy - consideration of epileptosurgical solution
- Compensation issue
In the examination request, it is necessary to state the address and telephone contact per patient. If the application is submitted by e-mail (preferred method), the applicant will be contacted by the coordinator, who will confirm receipt of the application and send the applicant a brief form to fill out. The application will then be assessed by a doctor and the applicant will be informed whether the patient has been placed on the waiting list, or with what priority. Please note that video-EEG monitoring is not an acute examination and the waiting time for it is approximately 3 months. The patient will be informed about the date of the examination by phone approx. 1 month in advance. At the same time, he will be sent detailed information about the course of the examination.
Location
The video-EEG monitoring unit is located in the adult section of FN Motol. Arrival is from node C / 2nd floor, I. neurology station. The examination is carried out in two above-standard equipped rooms with a separate bathroom, toilet, and television.
Operating time
24/7 (24 hours a day, 7 days a week).
Documents
They provide patient care
Doctors: MD David Krýsl, Ph.D., MD Adam Kalina, M.D. Petr Fábera, Ph.D., MD Hana Krijtová
Laboratory assistants: Pavla Kasíková, B.Sc. Lucie Kalinová, Renata Konečná Košová, Kateřina Šťovíčková, Hana Hulejová
Coordinator: Bc. Romana Lipinová
Nurses I. bed station
Contact
V Úvalu 84, Prague 5, 150 06
phone: 702
fax: +224 436 817 XNUMX
Email: epilepsie@fnmotol.cz
Chief physician: As. MD Radim Mazanec, Ph.D.
Station nurse: Alena Zdráhalová
Liquorological laboratory, phone number 224 436 870
EMG and EP laboratory, phone number 224 436 867
EEG laboratory, phone number 224 436 868
ENG laboratory, phone number 224 436 872
Neurosonological laboratory, phone number 224 436 874
Laboratory for the examination of the autonomic nervous system, phone number 224 436 872
Experimental laboratory of spatial cognition, phone number 224 436 879
Cerebrospinal fluid laboratory of the Institute of Immunology, 2nd Faculty of Medicine, Charles University and Motol University Hospital
It examines cerebrospinal fluid from adult and pediatric patients throughout the University Hospital in Motol, Na Františku Hospital and other external workplaces.
Cytological and biochemical analysis of cerebrospinal fluid is used mainly in the differential diagnosis of viral and bacterial neuroinfections, demyelinating diseases; particularly multiple sclerosis, in case of suspected subarachnoid hemorrhage, in cancers with infiltration into the cerebrospinal fluid and also clarifies the diagnosis of dementias, especially Alzheimer's disease.
Receipt of material is from 6-15 hours, tel .: 2443 6870/6871. Statimous cerebrospinal fluid examinations after 15 pm and on Saturday or Sunday are performed by the Immunology service in the pediatric part of the FNM, 4th floor. node G, tel.2443 2067. During the statim examination outside our laboratory, the laboratory assistant counts the elements in the F.-R chamber and makes a permanent specimen. Upon request, the company centrifuges, examines the Pandas and announces the result by phone.
Laboratory program
1.
Cerebrospinal fluid cytology (quantitative and qualitative)
The test is designed to determine the number of leukocytes and the differentiation of cell types in the cerebrospinal fluid. The examination is:
a) quantitative (determination of the number of leukocytes in the Fuchs-Rosenthal chamber)
b) qualitative (leukocyte differentiation in%)
Indications: suspected CNS inflammation, subarachnoid hemorrhage or meningeal cell infiltration.
2. Panda's reaction
Orientational evaluation of total protein concentration in cerebrospinal fluid.
principle: Protein precipitation with phenol solution.
3. Spectrophotometry
The examination is used to objectively detect xanthochromia in the cerebrospinal fluid due to the presence of blood pigment derivatives: Oxyhemoglobin (Oxy), bilirubin (Bi) and methemoglobin (Met).
Indication: Suspected subarachnoid fermentation (SAK)
4. Determination of immunoglobulin G (IgG) and albumin (Alb) in cerebrospinal fluid and serum and determination of permeability of the blood-brain barrier using albumin quotient (Q Alb)
The test is intended for the quantitative determination of immunoglobulin G (IgG) and albumin (Alb) in cerebrospinal fluid and serum by the immunonephelometric method. The assay is performed to calculate the IgG quotient (Q IgG) and the albumin quotient (Q Alb). Q Alb informs about the state of the blood-brain barrier.
5.Determination of IgM and IgA in cerebrospinal fluid and calculation of intrathecal synthesis of IgG, IgM and IgA according to Reiber graph
The values of Q IgG, Q IgM, Q IgA and Q Alb are fitted to the Reiber relation to determine the possible intrathecal synthesis of immunoglobulins of individual classes. At the same time, a graphical representation of the ratio of Q Alb and Q IgG in a Reiber diagram, which is part of the patient's output protocol, is performed. The test is intended for the quantitative determination of immunoglobulins M and A (IgM, IgA) in cerebrospinal fluid by the immunonephelometric method. Indication: diff. CNS inflammatory diseases.
6. Isoelectric focusing (IEF) of immunoglobulin G (IgG) in cerebrospinal fluid and serum
Examination demonstrates the presence or absence of IgG oligoclonal bands (OBs) in the patient's cerebrospinal fluid and serum. This determines possible intrathecal IgG synthesis in the central nervous system (CNS). The determination of OB is important especially in patients with suspected multiple sclerosis
7.
Cerebrospinal fluid laboratory:
RNDr. Jitka Hanzalová and laboratory assistant Eva Dudková
Office phone number: 244 368 70/6871
E-Mail: jitka.hanzalova@fnmotol.cz
Examination of antineural antibodies associated with autoimmune encephalitis and other central nervous system syndromes
How to apply for an examination?
- Fill it out electronic Application with the examination justification and the results of previous examinations (at least brain MRI, EEG, cerebrospinal fluid) to the e-mail address: neuroimmunologie@fnmotol.cz Printed Enclose the application with a stamp (including the ID number and expertise of the sending workplace and the name of the referring physician) with the samples. Fill it out Informed consent about the examination.
- Send samples: send coiled serum (red tube) (2ml) and (optimally also coiled) liquor (2ml) for examination. Samples must be sent in well sealed containers marked on behalf of a birth number patient, date of collection sample and clear indicating the type of sample (“Serum”, “cerebrospinal fluid”).
- Samples together with the application form and filled out Informed consent send to: Liquorology Laboratory of the Institute of Immunology of the 2nd Faculty of Medicine, UK and Motol General Hospital, Department of Neurology, 2nd Faculty of Medicine, UK and Motol General Hospital, V Úvalu 84, 150 06 Prague 6, phone: 22443 6870, 6871
The transport service must be informed that the samples must be handed over personally to RNDr. Hanzalové, or laboratory assistants Mr. Nosilová or Bc. Stychov.
We communicate the results to the referring physician and at the same time send them by post after final completion.
Due to capacity reasons, e-mail is used neuroimmunologie@fnmotol.cz exclusively for communicating with doctors.
Links:
- Request for antibody testing - please fill in the pdf, save and send to neuroimmunologie@fnmotol.cz and also send printed along with the sample
- Informed consent for antibody testing - please fill in with the patient and send together with the sample.
- Basic information on antineural antibodies associated with autoimmune encephalitides and other syndromes affecting the central nervous system (see attachment).
At FN Motol it is currently possible to investigate:
Known antigens on the commercial kits listed below
- PNP:
Panel of antibodies against onconeural antigens by line-blot method (anti-Hu, -Yo, -Ri, -Ma2 / Ta, -CV2 / CRMP5, -amphiphysin)
- PNP-GAD:
Panel of antibodies against onconeural antigens by line-blot method (anti-Hu, -Yo, -GAD65, -Ri, -Ma2, -Ma1, -CV2 / CRMP5, -amphiphysin, -Tr / DNER, -Zic4, -titin, -recoverin , -PKCɣ, -SOX1)
- AE mosaic:
Panel of antibodies against surface (membrane and synaptic) antigens by the method of indirect immunofluorescence on cells transfected for the given antigen (NMDAR, AMPAR1/2, GABABR, LGI1, CASPR2)
- anti-DPPX *
- anti-MOG
- anti-AQP4
- anti-IgLON5 *
Examination of tissue sections *:
- for intracellular antigens
- for surface antigens
It is used to detect the staining associated with the presence of an antibody against neuronal antigens in a given sample, which can be specified for a specific antigen by the methods mentioned above or to mediate confirmation in a research laboratory abroad. They are suitable for persistent clinical suspicion of an autoimmune disorder of the nervous system or to verify positivity on commercial kits.
*only by prior arrangement with doctors specializing in diagnostics (Martin Elišák, MD, Ph.D., Hana Mojžišová, MD)
Contact: neuroimmunologie@fnmotol.cz
Surgery hours Monday - Friday 8:30 - 15.
Tel. for ordering outpatients 224 436 867 (Lachmann, MD, Tuček, MD)
Tel. for ordering patients hospitalized in FN Motol line 6896 (As. MUDr. Mazanec, PhD)
Electromyography (EMG)
Functional examination method for the diagnosis of peripheral nervous system disorders (eg polyneuropathy, compression lesions (compression) of nerves in anatomical strains, traumatic nerve involvement or nerve entanglement, compression or injury of nerve roots in the spine, degenerative or inflammatory diseases of peripheral nerves), neuromuscular disorders transmission (eg myasthenia gravis, Lambert-Eaton syndrome) or muscle diseases (eg myopathy, myositis).
Electroneurography - stimulation of peripheral nerves by electrical impulses using a surface stimulation electrode, registration of responses from surface electrodes adhered either above the muscle or to the area of skin supplied by the relevant nerve. We use a ring electrode on the fingers of the upper limbs to register. This is a non-invasive examination.
Needle EMG - registration of responses from a needle electrode immersed in a muscle, first at rest, then at its contraction. This is an invasive examination.
Repetitive nerve stimulation - series of 10 electrical pulses with a frequency of 3 Hz using a surface stimulation electrode, registration of responses from surface electrodes glued above the muscle. This is a non-invasive test used in patients with suspected neuromuscular transmission disorders.
Repetitive nerve stimulation - series of 10 electrical pulses with a frequency of 3 Hz using a surface stimulation electrode, registration of responses from surface electrodes glued above the muscle. This is a non-invasive test used in patients with suspected neuromuscular transmission disorders.
No special preparation is required before the EMG examination, only before repetitive stimulation, cholinesterase inhibitors (drugs used to treat myasthenia) are discontinued if the patient is taking them. On the day of the examination, it is not recommended to apply greasy creams on the examined limbs, the limbs should be clean, freely accessible (eg not in plaster fixation). EMG cannot be performed if there is an acute inflammatory process at the test site. Swelling at the examination site reduces its informative value.
Evoked potentials
Investigation methods for functional evaluation of especially central pathways of various sensory modalities. The basic ones include evoked potentials (SEP), auditory (BAEP), visual (VEP) and motor (MEP).
SEP - with the help of electrical stimuli, the peripheral nerve on the upper or lower limb is stimulated, the responses of the cerebral cortex are sensed by means of an electrode cap placed on the head. We investigate sensitive pathways (conduction of sensitivity from the limbs through the spinal cord to the cerebral cortex), eg in patients with multiple sclerosis, with spinal cord involvement in degenerative and traumatic changes of the cervical and thoracic spine, or in neurodegenerative diseases.
BAEP - stimulates with a sound signal in the headphones, the answers are read from the back of the brain using electrodes glued behind the ears. We're investigating the auditory pathway. The examination can be used in patients with tinnitus, dizziness, or also in patients with suspected acoustic neurinoma (auditory nerve tumor).
Acts - Stimulation takes place by watching a television screen, where a changing image of the chessboard is projected, the answers are recorded from the cerebral cortex using an electrode cap on the head. We examine the visual pathway - most often in patients with retrobulbar neuritis (inflammation of the optic nerve) or visual disturbances of unclear cause).
MEP - stimulated with a magnetic coil placed on the head or above the cervical / lumbar spine, the answers are read by a surface electrode glued to the skin above certain muscles of the upper or lower limb. We examine the motor pathways from the cerebral cortex, where the command to move arises, through the spinal cord and peripheral nerve to the muscle. The examination is performed mainly in central movement disorders, eg in spinal cord compression in cervical / thoracic intervertebral disc herniation, in multiple sclerosis and in neurodegenerative diseases.
A standard EEG test is performed in the laboratory.
Location
The laboratory is located in the adult part of the Motol University Hospital, arrival is from node C or D / 2nd floor, part of the Clinic and Laboratory Management.
Working hours
Monday - Friday 7:30 - 15:00, acute examination until 18:00
Personnel
Laboratory assistants: Hana Hulejová, B.Sc. Lucie Kalinová, Pavla Kasíková, Kateřina Šťovíčková
Doctors: MUDr. David Krýsl, Ph.D., MD Hana Krijtová, MD Adam Kalina, M.D. Petr Fábera, M.D. Jana Kluhová, MD Vlastimil Šulc
Contact
V Úvalu 84, Prague 5, 150 06
phone: (224) 436 868
Email: eeg@fnmotol.cz
ENG laboratory
sister M. Jančíková
sister R. Rázková
Surgery hours Monday - Friday 8:00 - 15:00
To order, call the assistant on Mondays and Wednesdays between 10,00 and 12,00.
Phone 602 277 121 or email neuro.otologie@fnmotol.cz
You must have the recommendation of a neurologist, ENT doctor or RHB doctor for the examination, and you must also have an ENT certificate for an ear examination not older than 4 weeks (otoscopy).
ENG is an examination of the balance system, it takes about 1 - 1,5 hours. Do not drink coffee and other stimulant drinks, do not smoke or take any sedatives (ie painkillers) before the examination.
If you wear glasses, take them with you.
Welcome to our clinical and research laboratory!
Our laboratory is equipped with 2 ultrasonographic instruments: Toshiba Aplio 500 (transcranial, carotid, peripheral nerve and muscle probe, intraoperative) and Toshiba Nemio instrument with transcranial and carotid probe.
The examination can be ordered on tel. 224 436 874 from the head nurse of the counseling center Tereza Valentová Šípová.
The counseling center is open daily except Thursdays from 7:00 to 15:30.
Surgery hours Monday - Friday 8:30 - 15:30 according to order.
Your patients will be happy to examine and hopefully erudite:
doc. MUDr. Aleš Tomek, Ph.D., FESO, MUDr. Ivana Sarbochova, MD Martin Sramek, MD Jaroslava Paulasová Schwabová, Ph.D., MUDr. Hana Magerová, Ph.D.
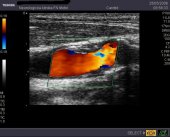 Duplex examination of extracranial sections of arteries supplying the brain
Duplex examination of extracranial sections of arteries supplying the brain
We examine the carotid basin in a standard way (CCA, ICA, ECA), but we supplement it with a transcranial probe examination (ICA under the base inaccessible to the carotid probe, course through the carotid siphon, collateral flow - a. Ophthalmica, Willis circuit status). We also examine the cervical segment of the vertebral artery (also supplemented at the discretion by TCCS examination intracranially).
Transcranial color sonography, TCCS
The examination will provide orientation information about the basic properties of the brain parenchyma (midline shift, ventricular system) and detailed information about the cerebral arteries of the Willis circuit (diameter, shape anomalies) and their flow parameters (stenosis detection, occlusion). We show the intracranial section of the carotid artery 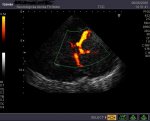 internal (including siphon course), a. ophthalmic, a. cerebri media (M1-M3 segment), a. cerebri anterior (A1-2), a. cerebri posterior (P1-2), a. basilaris, intracranial sections a. vertebralis and, with good investigability, also smaller arteries of the VB circulation (PICA, AICA, SCA).
internal (including siphon course), a. ophthalmic, a. cerebri media (M1-M3 segment), a. cerebri anterior (A1-2), a. cerebri posterior (P1-2), a. basilaris, intracranial sections a. vertebralis and, with good investigability, also smaller arteries of the VB circulation (PICA, AICA, SCA).
The indication of the examination is a suspicion of arterial brain disease. The most severe is the evidence of cerebral artery disease (atherosclerotic, vasculitis), less useful is the detection of vascular anomalies (aneurysms, AV malformations, vascularized tumors), where it serves only as a rough guide and does not represent CTAg, MRA or DSA.
Transcranial Doppler sonography, TCD
This classic examination is fully replaced by TCCS, at the indication of TCD we will supplement the complete TCCS, which will also provide structural data and provide the examiner with a better overview of the possible pathology of vascular flow.
Right-left short circuit detection
The test requires the introduction of a contrast agent (hydroxyethyl starch solution with microbubbles) into a vein. The ultrasound examination is then performed at rest and during the so-called Valsalva maneuver (clenching of the abdominal muscles).
Determination of cerebrovascular reserve capacity (vasomotor reserves)
The examination is indicative of the state of cerebral perfusion. It is indicated especially when closing the internal carotid artery. The patient holds their breath during the examination and we test how holding their breath affects brain perfusion.
Positional tests on the vertebral artery
The examination takes place in different positions of the head - for example, maximum rotation and tilt of the neck to one side and then to the other side. It makes it possible to determine whether the cerebral artery is not calmed down by the cervical vertebrae in one of the extreme positions.
Detection by microembolization into CNS arteries
The examination consists of a longer resting measurement of brain flow and detection of microembolization signals. It does not require the insertion of a peripheral cannula.
Monitoring of interventions (carotid stenting, thrombolytic therapy)
These examinations are not available to outpatients, we perform them only as indicated during hospitalization.
The Department of Neurology of the 2nd Medical Faculty of Charles University is a continuation of the tradition of the neurological department of the Motol University Hospital, founded in 1957.
At the birth of Motol neurology was MUDr. F. Hanzal, then an associate professor at the Henner Neurological Clinic, who since 1953, as a neurological consultant, provided all the neurological care for the town hospital in Motol.
In 1957, a neurology department was established in the Motol hospital, which was initially significantly contributed to by MUDr. S. Káš and MUDr. J. Orzságh.
In the sixties, prof. MUDr. K. Mathon, next to doc. MUDr. Hanzala another of the famous Czech neurologists.
After Mathon's death, prof. MUDr. F. Hanzal, DrSc., A recognized expert in the field of neuroinfections and cerebrospinal fluid examination. Prof. In 1976, Hanzal left for the position of Head of the ILF Neurological Clinic in Krč.
Doc. MUDr. H. Krejčová, DrSc., Who ran the clinic from 1976 to the end of 1992 and focused mainly on the development of vestibulological and electrophysiological laboratories and research on balance disorders at the European level.
From 1993 to November 2012, the head of the clinic was prof. MUDr. M. Bojar, CSc. Together with his colleagues, he developed the best traditions of the Czech and Slovak schools of neurology, especially in the field of care for patients with inflammatory nervous system disorders.
Since November 2012, the head of prof. MUDr. P. Marusič, Ph.D.
Our clinic is confirmed by the Ministry of Health of the Czech Republic as an accredited workplace for postgraduate teaching of neurology, neurology in preparation for certification and for neurological internships in other fields in preparation for the relevant field certification.
The clinic organizes postgraduate courses focused on teaching epileptology, electrophysiological examination methods (EEG, EMG, EP) and vestibulology.
Contact for those interested
Prim. doc. MUDr. Aleš Tomek - tel. 224 436 803
PhDr. Daniel Jirkovský, Ph.D., MBA - Head of the Independent Education Department of the Motol University Hospital, tel. 224 439 030
On May 30, 2014, the reconstruction of the equipment of the waiting room of our clinic was completed, which was carried out with the help of the association Design Help, os for hospitable. Thank you so much!
The purpose of video-EEG monitoring is to evaluate typical seizures of the patient. The examination will help determine if the seizures are and what type they are, or if they are of a different nature.
If surgical treatment of epilepsy is being considered, the examination will help determine in which area of the brain the seizures occur. As part of the preoperative examination, the so-called invasive Video-EEG monitoring with intracranially implanted electrodes.
The examination makes it possible to assess whether epilepsy is compensated and whether unobserved or so-called subclinical seizures do not occur. Answering any of these questions may affect further treatment.
Ordering for video-EEG monitoring
It is possible to order a patient for the examination in writing or by email.
The doctor indicating the examination will send a request for an examination to the address of the center detailed report about the patient and the formulated question that this examination should solve:
- Differential diagnosis of epileptic and non-epileptic seizures
- Determination of the type of epileptic seizures
- Drug-resistant epilepsy - consideration of epileptosurgical solution
- Compensation issue
It is necessary to state in the request for examination address a telephone contact on the patient. The patient will be informed of the date of the examination by telephone and then in writing with detailed information on the course of the examination.
In most cases, the examination is not acute, the waiting period is approximately 2-3 months. In indicated cases, it is possible to individually arrange a priority assignment for examination.
Location
I. bed station
Documents
Questionnaire for patients with seizure disorders
Contact
fax: +224 436 820 XNUMX