- Basic information
- Management and staff
- Ambulance
- Inpatient wards
- Clinic specialization
- TRAUMA
- History
- Information for patients
- Information for patients with plaster bandage
- Hallux valgus
- Hallux rigidus
- Teaching, Education
- Master's degree
- Optional subjects
- Elective subjects
- Gallery
- Contact


I. orthopedic clinic of the 1st Medical Faculty of Charles University and University Hospital Motol
Orthopedics and traumatology of the musculoskeletal system with a focus on:
- large joint replacements, especially complicated conditions after birth defects, injuries, systemic diseases and revision surgeries
- Traumatology
- rheumatic surgery
- solution of complicated post-traumatic conditions of the musculoskeletal system
- arthroscopic joint defects and injuries
- surgical treatment of tumors of the musculoskeletal system
- problems of bone and joint infections and especially the solution of joint replacement infections
- hand surgery
- surgical treatment of congenital and acquired foot defects
- development of original joint replacements
The head
Prof. MD Ivan Landor, CSc.
(224) 433 901
Secretariat
224 433 901 - not used for ordering patients
contact e-mail: renata.roubalova@fnmotol.cz
Patient ordering
card file: (224) 433 925
We only order patients with a referral from a peripheral orthopedist with an indication for surgery.
Location:
Motol University Hospital
SECRETARIAT
ground floor of the main building, connecting corridor B - C - Complement
AMBULANCE
ground floor of the main building, NODE B
V Úvalu 84
150 06 Prague 5
The head
- Prof. MD Ivan Landor, CSc.
tel.: 224 433 901
Primary
- Prof. MD Stanislav Popelka, CSc.
phone: 224 433 903
Email: stanislav.popelka@fnmotol.cz
Head nurse
- Petra Sklenářová DiS.
tel.: 224433905
Email: petra.sklenarova@fnmotol.cz
Professors
- Prof. MD David Jahoda, CSc.
- Prof. MUDr. David Pokorny, CSc.
- Prof. MD Stanislav Popelka, CSc.
- Prof. MUDr. Antonin Sosna, DrSc.
Teachers
- Doc. MD Petr Fulín, Ph.D., MBA
- Doc. MD Jan Pech, CSc.
- Doc. MUDr. Vera Pinskerova, Ph.D.
- Doc. MUDr. Rastislav Hromadka, Ph.D.
- Doc. MD Vladislav Barták, Ph.D.
Professional assistants and staff
- as. MD Evžen Beitl, Ph.D.
- as. MD Pavel Belán
- as. MD Zdeněk Borský
- as. MD Pavel Dupal
- as. MUDr. Jan Dobias
- as. MD Kristián Güttler, Ph.D.
- as. MD Jan Hach
- as. MD Jaroslav Kalvach
- as. MD Tomas Kruta
- as. MD Miroslav Netval, CSc.
- as. MD Milan Richter, CSc.
- as. MD Jan Valenta, CSc.
- as. MD David Veigl, Ph.D.
- as. MUDr. Martin Vlcek, Ph.D.
- as. MUDr. Tomas Zatrapa
Doctors
- MD Rastislav Ballay
- MD Miloš Barna
- MUDr. Jindrich Bartak
- MD Jiří Bek
- MD Viktor Bezvoda
- MD Otakar Dosoudil
- MD Milan Hein
- MD Karel Hejno
- MD Jan Heřt
- MUDr. Zdenka Honzova
- MD Aneta Rybáková
- MD Michal Koutek
- MD Pavel Kubicek
- MD Petr Libanský
- MD Edib Jaganjac
- MD Marek Jokl
- MUDr. David Jonas
- MUDr. Tobias Judl
- MD Robert Manek
- MD Matej Mazura
- MUDr. Pavel Melichercik, Ph.D.
- MD Pavel Mišek
- MD Marek Niedoba
- MD Jannis Papadopoulos
- MD, Jiří Polák
- MUDr. Stanislav Popelka Jr.
- MD Zdenek Šmidl
- MD Stanislav Stefanisko
- MD Jan Štědrý
- MD Roman Stícha
- MD Jan Tomades
- MD Milan Valcha
- MD Jiří Walder
Blue pavilion, part for adults
Ground floor, communication node B
Office hours: Mon-Fri 8:00-15:00
Patients can make an appointment via file cabinets:
Card file Traumatology - 224 438 624 Mon-Fri 8:00-15:00
Email: traumatologie@fnmotol.cz
Card file Orthopedics - 224 433 925 Mon-Fri 12:00-15:00
Email: 1.ortopedie@fnmotol.cz
E-mails are only used for ordering already registered patients - choose this option first. Enter the information required for ordering in the message.
New patients we order only with a recommendation from a peripheral orthopedist with an indication for surgery - for the first order of an examination, choose telephone or personal contact.
It is not possible to answer questions about your state of health, recommend or otherwise consult a treatment procedure, or arrange an alternative surgery date via e-mail.
For results and consultations, please call the clinics of the respective doctors.
If the patient is not insured, it is necessary to contact them first Foreign and Private Patient Department - 224 443 681, 224 443 682.
Monday
| Ambulance No. 1 (224) 433 973 | MD Roman ŠTÍCHA S. A. Hykešová |
| Ambulance No. 2 (224) 433 974 | MD Jiří BEK s. L. Matková |
| Ambulance No. 3 (224) 433 975 | MD Milan HEIN - 1x in 14 days s. M. Adámková |
| Ambulance No. 4 (224) 433 976 | MD Tobias JUDL s. J. Pejčochová |
| Ambulance No. 5 (224) 433 978 | Prof. MD Ivan LANDOR, CSc. s. L. Kurková |
| Ambulance No. 6 (224) 433 930 | MD Rastislav BALLAY s. L. Kurková |
| Ambulance No. 7 (224) 433 977 | MD David JONÁŠ s. L. Kurková |
| Traumatology ambulance No. 1 (224) 438 627 | MD Jaroslav KALVACH, s. J. Horká |
| Traumatology ambulance No. 2 (224) 438 662 | MD Robert MANEK s. I. Huňáčková |
| Traumatology ambulance No. 3 (224) 438 626 | MD Pavel MÍŠEK s. J. Poláčková |
Tuesday
| Ambulance No. 1 (224) 433 973 | MD Pavel DUPAL, MBA s. L. Matková |
| Ambulance No. 2 (224) 433 974 | MD David VEIGL, Ph.D. s. J. Pejčochová |
| Ambulance No. 3 (224) 433 975 | MD Jan HACH s. H. Kopernická |
| Ambulance No. 4 (224) 433 976 | MD Petr LIBÁNSKY s. M. Adámková |
| Ambulance No. 5 (224) 433 978 | Doc MUDr. Rastislav HROMÁDKA, Ph.D. s. L. Kurková |
| Ambulance No. 6 (224) 433 930 | MD Matej MAZURA s. L. Kurková |
| Ambulance No. 7 (224) 433 977 | MD Milan RICHTR, CSc. |
| Traumatology ambulance No. 1 (224) 438 627 | MD Evžen BEITL, Ph.D. s. J. Horká |
| Traumatology ambulance No. 2 (224) 438 662 | MD Pavel BELÁN until 11:00 a.m s. I. Huňáčková |
| Traumatology ambulance No. 3 (224) 438 626 | MD Marek JOKL s. J. Poláčková |
Wednesday
| Ambulance No. 1 (224) 433 973 | Prof. MD Stanislav POPELKA, CSc. s. M. Adámková |
| Ambulance No. 2 (224) 433 974 | MD Vlastislav BARTÁK, Ph.D. pp. I. Smooth |
| Ambulance No. 3 (224) 433 975 | MD Pavel DUPAL, MBA s. L. Matková |
| Ambulance No. 4 (224) 433 976 | Doc. MD Věra PINSKEROVÁ Ph.D. s. J. Pejčochová |
| Ambulance No. 5 (224) 433 978 | Prof. MD Antonín SOSNA, DrSC. s. L. Kurková |
| Ambulance No. 6 (224) 433 930 | Doc. Petr FULÍN, Ph.D., MBA s. L. Kurková |
| Ambulance No. 7 (224) 433 977 | MD Jan HEŘT s. L. Kurková |
| Traumatology ambulance No. 1 (224) 438 627 | MD Zdeněk ŠMÍDL until 11:00 a.m s. J. Horká |
| Traumatology ambulance No. 2 (224) 438 662 | MD Marek NIEDOBA s. I. Huňáčková |
| Traumatology ambulance No. 3 (224) 438 626 | MD Martin VLCEK s. J. Poláčková |
Thursday
| Ambulance No. 1 (224) 433 973 | Doc. MD Jan PECH, CSc. s. H. Kopernická |
| Ambulance No. 2 (224) 433 974 | MD Kristián GÜTTLER, Ph.D. with L. Matková |
| Ambulance No. 3 (224) 433 975 | MD Tomas TURKEY with Z. Charouzková |
| Ambulance No. 4 (224) 433 976 | MD Pavel MELICHERČIK s. J. Pejčochová |
| Ambulance No. 5 (224) 433 978 | MD David VEIGL, Ph.D. s. M. Adámková |
| Ambulance No. 6 (224) 433 930 | MD Jiří BEK s. M. Adámková |
| Ambulance No. 7 (224) 433 977 | MD Tomáš ZATRAPA S. A. Hykešová |
| Traumatology ambulance No. 1 (224) 438 627 | MD Otakar JUDGED s. J. Horká |
| Traumatology ambulance No. 2 (224) 438 662 | MD Edib JAGANJAC s. I. Huňáčková |
| Traumatology ambulance No. 3 (224) 438 626 | MD Miroslav STRECK s. J. Poláčková |
Friday
| Ambulance No. 1 (224) 433 973 | MD Jan VALENTA, CSc. pp. I. Smooth |
| Ambulance No. 2 (224) 433 974 | MD Miroslan NETVAL CSc. s. H. Kopernická |
| Ambulance No. 3 (224) 433 975 | MD Zdeněk BORSKý sister Z. Charouzková |
| Ambulance No. 4 (224) 433 976 | MD Jan DOBIÁŠ s. L. Matková |
| Ambulance No. 5 (224) 433 978 | Prof. MUDr. David JAHODA, CSc. s. M. Adámková |
| Ambulance No. 6 (224) 433 930 | MD Jan ŠTĚDRÝ s. M. Adámková |
| Ambulance No. 7 (224) 433 977 | MD Jan TOMAIDES s. J. Pejčochová |
| Traumatology ambulance No. 1 (224) 438 627 | MD Milan VALCHA s. J. Horká |
| Traumatology ambulance No. 2 (224) 438 662 | MD Karel HEJNO s. I. Huňáčková |
| Traumatology ambulance No. 3 (224) 438 626 | MD Jindřich BARTÁK s. J. Poláčková |
Blue Pavilion, adult part:
- 1st ward: node B, ground floor – 30 beds, phone: 224 433 933
Leading physician: Doc. MD Petr Fulín, Ph.D., MBA
Station nurse: Lucie Kopernická
- 2st ward: node B, 1st floor – 3 beds, phone: 224 433 934
Chief physician: As. MUDr. Kristián Güttler
Station nurse: B.Sc. Tomas Walla
- 3st ward: node C, ground floor – 30 beds, phone: 224 433 935
Chief physician: as. MD Tomáš Zatrapa
Station nurse: Mgr. Daša Klívarová
- Septic department: node C, - ground floor – 20 beds, phone: 224 433 989
Leading physician: doc. MD Vladislav Barták, Ph.D.
Station nurse: Martina Hatáková
- 4th inpatient department: node C, -2. floor – 30 beds, phone: 224 438 630
Chief physician: MUDr. Milan Valcha
Station nurse: Jana Veselá
- Traumatological ICU: node B, 2st floor – 12 beds, phone: 224 438 638
Chief physician of the trauma department: As. MUDr. Evžen Beitl, Ph.D.
Chief physician of the orthopedic part: As. MUDr. Zdeněk Borský
Station nurse: Romana Šišková, DiS.
- Orthopedic ICU: node B, 1st floor – 4 beds, phone: 224 433 940
Chief physician: As. MUDr. Kristián Güttler
Station nurse: B.Sc. Tomas Walla
Orthopedics and traumatology of the musculoskeletal system with a focus on:
- large joint replacements, especially complicated conditions after birth defects, injuries, systemic diseases and revision surgeries
- Traumatology
- rheumatic surgery
- solution of complicated post-traumatic conditions of the musculoskeletal system
- arthroscopic joint defects and injuries
- surgical treatment of tumors of the musculoskeletal system
- problems of bone and joint infections and especially the solution of joint replacement infections
- hand surgery
- surgical treatment of congenital and acquired foot defects
- development of original joint replacements
Traumatology part of the Orthopedic Clinic of the 1st Medical Faculty of Charles University and the University Hospital Motol
The care of patients with injuries has its professional and operational specifics. In addition to professionalism, the ability to make immediate decisions is also important in traumatology. At the Orthopedic Clinic of the First Medical Faculty of Charles University and the Faculty of Medicine, great attention is paid to traumatology. A specialized team of paramedics provides the necessary health care in the departments of accident reception, standard and intensive care, and emergency operating rooms.
Accident income
There are 6 examination beds on which, in cooperation with other clinics, patients not only with injuries to the musculoskeletal system, but also with injuries to the head, chest and abdomen are treated. The operation is non-stop, 24 hours a day.
Patients with the most serious injuries are treated on the so-called "Traumabox". The ambulance is specially equipped for rapid diagnosis and treatment of patients, including resuscitation. The location of the traumabox is connected to the complex of urgent operating theaters.
In the past year, more than 31 patients with various serious injuries were treated on the "accident intake". When accepting patients from the emergency services, a system of "advised income" is used for quick and uncomplicated transfer. Accident ambulances are designed for acute treatment. After urgent treatment, patients requiring further professional outpatient care are referred to the relevant outpatient clinics according to the type and severity of the injury, taking into account the place of residence.
The operation at the accident reception is subject to urgent, unplanned treatment and the order of patients is governed by the severity of the injury.
Hospitalization
Hospitalization takes place in standard and intensive care beds. Currently, there are 30 standard beds for injuries, of which 3 beds (2 rooms) are with above-standard equipment. Another 8 beds are available in the intensive care unit. Around 2000 patients are hospitalized annually. Follow-up nursing and rehabilitation care for patients, in the vast majority of seniors, is often long-term and is handled in cooperation with the social department of the National Hospital. If the patient's state of health does not allow for home care, rehabilitation or social follow-up care is offered at the FNM or at other health care providers. We cannot provide long-term care on the beds of the I. Orthopedic Clinic.
Operating rooms
More than 1500 patients are operated on in emergency rooms each year for injuries. My most common operations are operations for a fracture of the upper end of the femur. In these patients, depending on the type of fracture, the choice is between rescue surgery with osteosynthesis or implantation of a hip replacement.
The number of treated and hospitalized patients with an accidental diagnosis in the FNM is constantly growing. This is also because the University Hospital in Motol has gained the status of the highest level of trauma center.
Education
Trauma doctors participate in undergraduate and postgraduate education. A new syllabus of internships and seminars on traumatology is currently being prepared. Interested students of medical faculties can, in agreement with the management of the clinic, practice on an accident basis.
Volunteer program
You can also meet "volunteers" in our departments. If you want to help our patients and you are interested in volunteering, please contact the "Volunteer Center FNM". Thank you.
While the 1st clinic founded in the Czechoslovak Republic was the Bratislava Clinic, whose founder was prof. Chlumský, is the first orthopedic clinic of Charles University in Prague, the first and oldest established orthopedic clinic in the Czech lands. This clinic was founded by prof. Stanislav Tobiášek in 1.
Prof. MUDr. Stanislav Tobiášek, first head of the 1st Orthopedic Clinic in Prague Prof. Tobiášek has been interested in orthopedics since he worked at the surgical clinic with prof. Maydla and later prof. Kukuly. He deepened his knowledge with prof. Lange in Munich and prof. Lorence in Vienna. He gained his first very valuable surgical experience during the Balkan Wars, when he worked in a military hospital under the leadership of prof. Fir trees. For his work he received from King Peter of Serbia the Order of St. Sava III. degrees. He was habilitated in 1909 by prof. Kukulou. Unfortunately, he had many enemies under Austria, he was called "politisch verdächtig und unverläslich". His proposed extraordinary professorship was held in Vienna for many years. After the First World War, Tobiášek was appointed associate professor and was promised that he would receive premises for an orthopedic clinic. At that time, in 1927, the Orthopedic Clinic was defacto, one of the departments of the 2nd Surgical Clinic, which did not provide enough opportunities and space for the newly emerging and newly profiled field of orthopedics. The incompetent superior authorities eventually called on Tobiášek to find suitable premises for the orthopedic clinic himself. After longer negotiations, prof. With the help of his friend the architect Hübschmann, who prepared free plans for the reconstruction of the old Merchant's Hospital and managed the construction for free, Tobiášek finally managed to open the first orthopedic clinic in the Czech Republic. This is how complicated the first independent orthopedic clinic in the Czech lands was established, in Ke Karlovu Street, Prague 2. |
The building of the so-called old Merchant Hospital after reconstruction into the first seat of the 1st Orthopedic Clinic in Prague 2, Ke Karlovu Street The clinic dealt mainly with conservative treatment of musculoskeletal disorders and included a bandaging and prosthetic workshop. |
Prof. Tobias at work in a prosthetic workshop Very few surgical procedures were performed and the main procedures were osteoclasia and simple tenotomies or incisions of musculoskeletal abscesses and empyema. After the death of prof. Tobiášek briefly managed the clinic of Dr. Polívka, which was in 1933. The end of 1933 became a major turning point in the activities of the clinic, when prof. Zahradníček was appointed head of the 1st Orthopedic Clinic. |
Prof. MUDr. Jan Zahradnicek, DrSc. A new era of Czechoslovak orthopedics dates from this year. Prof. Zahradníček is an extraordinary figure in Czech orthopedics and is undoubtedly the founder of the modern field of operations. Prof. Zahradníček was born on June 13, 6 in the Bohemian-Moravian Highlands in Mastník, which is a small Moravian village southwest of the district town of Třebíč. After studying at the grammar school in Třebíč, he decided to study at the Czech Medical Faculty of Charles University in Prague, which he graduated on March 1882, 27. After graduating, he worked briefly as an external specialist at the internal clinic of prof. Thomayer, he also went through other departments and finally on April 3, 1909 he became the operating election at the surgical clinic of prof. Kukuly. Due to his abilities, he received the position of assistant on October 1 of the same year. However, the events of the war (Balkan wars) lead him to work in a military hospital in Belgrade. During the Second Balkan War, he worked as a chief surgeon in Sofia, Bulgaria, where he treated and mainly operated until the end of August 4. After returning to Kukula's clinic, however, World War I soon broke out and from the end of June 1910 until the end of October 1, Zahradníček Commander of the 10st Surgical Group prof. Balls on various battlefields (near Tarnów, Gorlice, Zakliczin, Nadbrzesse and Rozvadov). He later worked in Albania and returned to Kukula's clinic after the end of the war. His work as a war surgeon brought him a wealth of experience and gave him what his students always remembered with admiration - the ability to make quick decisions, to choose a straightforward solution in surgical technology and the most logical path to success. Zahradníček briefly works at the Masaryk University in Brno in surgery prof. Petřivalský. Prof. for the field of orthopedics has already become prof. In 2 and 1913, Kukula expanded his habilitation from orthopedics to an associate professor of surgery. In June 1, the dean's office of the Faculty of Medicine of Charles University called doc. Gardener to Prague. A place became vacant after the deceased prof. Rudolf Jedliček, who led II. surgical clinic. In 1914, when prof. Stanislav Tobiášek, the life mission of prof. Zahradníčka, who after a short time, when the clinic - as we have already mentioned - was run by dr. As a full professor at Charles University, Polívka becomes its second head. Prof. Zahradníček is gradually developing intensive operational activities and introducing his priority operational techniques. He became famous for his own method of treatment of congenital dislocation of the hip joint, he is the discoverer of the so-called derotation principle in the treatment of this defect, but he also became famous for joint surgery, he also had his own external fixator for the treatment of infected fractures, etc. Another era in the activities of the 1st Orthopedic Clinic is the end of World War II, when the 2st Orthopedic Clinic was relocated to the building of the former Schneider Sanatorium in Na bojišti Street, Prague 1. |
The building of the 1st Orthopedic Clinic in Prague 2, Na bojišti Street It is interesting that the clinic was handed over by prof. Zahradníček Josef Smrkovský, who died shortly after the invasion of Soviet troops during the Prague Spring as a politician who had already been written off at the time, in the first orthopedics of the pelvic chondrosarcoma. Prof. Zahradníček ran the clinic with a firm hand until his death until October 1, 12. His death was preceded by participation in an orthopedic congress in Moscow, where he received the introductory lecture enthusiastically received by all participants. Unfortunately, he became ill in Moscow and was treated for alleged pneumonia. As soon as he felt better, he immediately went home, but he could see the change. He did not feel well, although he went to the clinic regularly. It is probable that he already had an undiagnosed myocardial infarction in Moscow, on the recurrence and consequences of which he died. The profile of Zahradníček's clinic covered practically the entire spectrum of orthopedic surgery performed at that time. However, the basis was undoubtedly the operation of congenital dislocation of the hip joint and its consequences. |
Prof. Gardener during the operation of congenital dislocation of the hip joint Zahradníček supported all capable assistants and gave them space for further development of the field. His first assistant, dr. Čížek, already started. In the 50s, he began to deal with the issue of joint sculptures, performed a number of experiments using osacrylic as an interposition sculpture, and introduced the operation of Judet's osacrylic caps and interposition sculptures according to Austin - Moore. In addition to the first assistant, Dr. Čížka, was an extraordinary personality of the clinic MUDr. František Stryhal, to whom, however, the communist regime gave the professorship as maximum recognition, so he did not receive his well-deserved professorship until after the revolution. |
Doc. During his time at the clinic, Stryhal was undoubtedly the most literate and educated figure in orthopedics. With her friend prof. Tošovský, who was also briefly one of the assistants of prof. Zahradníčka, wrote an important work "Children's Fractures", which served many generations of orthopedists as a basic textbook of pediatric traumatology of the musculoskeletal system. Among other extraordinary personalities of the 1st Orthopedic Clinic, it is necessary to name doc. MUDr. Jaroslav Slavík, CSc., Who later became the head of the orthopedic clinic in Pilsen, MUDr. Aleš Ondrouch, CSc., MUDr. Miroslav Lomíček, who was the first at the clinic to deal with scoliosis, MUDr. Maria Benešová, who successfully devoted herself to the conservative treatment of congenital hip arthroplasty using the biomechanical apparatus of prof. Hanauska. |
Prim. MD Hanausek Other Zahradníček's pupils from this 1st era were MUDr. Seidl, who went to the primary office in Kladno and founded a well-functioning orthopedic and trauma department, Prim. MUDr. Lukeš, who founded and led orthopedics in Teplice for years and MUDr. Procházka, who founded the orthopedic department in České Budějovice. In prof. Zahradníčka also worked briefly for prof. Hněvkovský - later founder of the 2nd Orthopedic Clinic, prof. Kubát, who for some time ran the 2nd orthopedic clinic, MUDr. Hořák - later head of the orthopedic department in Písek, MUDr. Matějka, who later worked as a primary in Příbram, MUDr. Miloš Kofroň - an honest classical orthopedist who later worked at the polyclinic on Charles Square. One cannot help but remember the first Czech radiologist who focused on the diagnosis and therapy of the musculoskeletal system and who headed the X-ray department of the clinic - MUDr. Antonín Sosna the Elder. |
Joint photo of prof. The gardener and his pupils from the 50s Zahradníček's last real student was MUDr. Oldřich Čech, who later became the head and founder of the Orthopedic Clinic of the 3rd Medical Faculty of Charles University in Vinohrady. MUDr. Oldřich Čech gained his orthopedic and traumatological experience with MUDr. Seidla at the orthopedic-traumatological department of the hospital in Kladno. Since 195 he has been actively participating in seminars with prof. Zahradníčka, who then admits him to the 1st Orthopedic Clinic. As can be seen from this brief list, the students of prof. Zahradníčka covered a professionally and geographically large piece of Czech orthopedics. As confirmed by all students prof. The gardener's atmosphere at the clinic was remarkable for its friendly spirit, which, despite the great respect aroused by the personality of the great boss, had an extraordinary effect on everyone. Everyone remembers this time as the years when the great boss passed on his experience to them and still left them full space to develop their personality and fulfill their professional interests. After the death of prof. Zahradníčka became the head of the 1st orthopedic clinic prof. MUDr. Miroslav Jaros, DrSc. |
Prof. MUDr. Miroslav Jaros, DrSc. The era of his work is unfortunately characterized by the growing influence of communist ideology, which prof. Jaroš was no longer able to defend himself. He himself was an extraordinarily educated orthopedist with extensive knowledge, but operationally he was significantly less active than his predecessor. However, he did not prevent capable clinic assistants from being educated and introducing new methods into the clinic's operating repertoire. At the time of his work, doc. MUDr. Emil Eis, CSc., Who became the head of the clinic after him. He also worked here. MUDr. Jiří Náhoda, CSc. - later professor and head of the Pilsen Orthopedic Clinic. MUDr. Milos Gregar, MD Jan Dvořák and other above-mentioned direct students of Zahradníček. We consider MUDr. Zdeněk Matějovský, who later became the founder of modern Czech oncology of the musculoskeletal system and, as a professor and doctor of science, became the head of the ILF clinic in Bulovka after the revolution. Not to mention MUDr. Stanislav Malkus, who became the head of the regional prosthetic department and his successor MUDr. Bohuslav Vrbický. The most important assistant of the clinic at that time was MUDr. Oldřich Čech, CSc., Who received recognition only after the change of the political regime, became a professor, doctor of science and had the opportunity to establish an orthopedic clinic of the 3rd Medical Faculty of Charles University in Vinohrady. Prof MUDr. Oldrich Cech, DrSc. is after prof. Undoubtedly, Zahraníček is the greatest figure in Czech orthopedics. During his stay at the clinic in St. Galena and prof. Müller and later BG Weber gained great experience and ingenious principles of the Swiss operating school, which he further developed, enriched with his own ideas and developed upon his return to our country. As a member of the ČSOT committee, he was appointed chairman of the technical commission at the ČSOT committee in 963. Thanks to him, Czech orthopedics soon had the opportunity to introduce a method of stable osteosynthesis in the treatment of fractures and joints, whether internal or external fixation, and in 1970 it saw the emergence of the first Czech hip replacement, which O. Čech developed with his colleagues in then SONP Poldi Kladno. Prof. The Czech Republic was not only able to co-create and ensure the production of instruments and implants, but also managed to put these groundbreaking modern methods into practice throughout the Czechoslovak Republic. |
As. MUDr. Oldrich Cech, CSc. with MUDr. A. Sosná jr. When bandaging a patient treated with Čech's external fixator for femoral joint In the era of prof. Jaroš was also joined by MUDr. Vratislav Rybka and MUDr. Antonín Sosna junior, whom you as. MUDr. O. Čech, CSc. he initially chose as his disciple and soon as his collaborator. MUDr. Miroslav Slavík, who in 2 got the position of ILF assistant and later after prof. Pavlanský took over the management and leadership of the ILF orthopedic clinic in Bulovka and was appointed professor after the habilitation. Prof. Due to his age, Jaroš was replaced in the management of the clinic by doc. MUDr. Emil Eis, CSc., Who has run the clinic since 1970. |
Doc. MD Emil Eis, CSc. Prof. Jaroš then died in his office at the clinic this year, perhaps after an asthma attack. The era of doc. Eise is unfortunately marked by the political influences of the so-called normalization, for the clinic there is undoubtedly a great loss the fact that doc. MUDr. Stryhal, DrSc. he was not allowed to run the clinic and that this extraordinary orthopedist was not given the space he deserved for his work. The company. MUDr. O. Čech, CSc., Who did not have the opportunity to habilitate at that time, and received his habilitation and professorship many years later. Nevertheless, thanks to his immense energy, he was in fact the leading figure of the clinic, where he introduced all the avant-garde methods he had acquired during his long stays in Switzerland. At that time, as already mentioned, he chose MUDr. A. Sosna jr., Who, due to his anatomical anamnesis (he was the last medical student of Prof. Borovanský), contributed to the development of surgical techniques and new surgical approaches. After the departure of doc. MUDr. Eise, CSc. doc. was appointed head of the clinic. MUDr. Vratislav Rybka, CSc., Who soon defended his doctorate and became a professor. |
Prof. MD Vratislav Rybka, DrSc. Prof. Rybka focused very soon thanks to the help of prof. MUDr. Stanislav Popelka, DrSc., Who opened the way for him, to the issue of rheumatic surgery. At that time, the era of cooperation with the Research Institute of Rheumatic Diseases began. Prof. After returning from a study stay in Heinol, Finland, Rybka introduces aloplasty of the knee joint into the clinic's repertoire and seeks a way to secure a Czech manufacturer for this implant. He succeeds in opening cooperation with Walter-Motorlet and in a team of other collaborators to develop the first Czech Walter-Motorlet knee replacement in 1984. Since then, the operation of another joint replacement - knee replacement - has been developing successfully. However, it is not just that the MUDr. Pavel Vavřík and MUDr. Ivan Landor, with whose help the first uncemented Walter-Motorlet hip replacement was created in 1988. In 1984, doc. MUDr. Oldrich Cech, DrSc., MUDr. A. Sosna, CSc., MD M. Krbec, MD T. Trč and MUDr. J. Vávra and help the new head to establish an orthopedic clinic of the 3rd Medical Faculty of Charles University in Vinohrady. Doc. MUDr. Martin Krbec, CSc. later became the head of the Orthopedic Clinic in Brno-Bohunice and doc. MUDr. Tomas Trc, CSc. becomes the head of the Orthopedic Clinic for Children and Adults, 2nd Faculty of Medicine, Charles University, FNM. In 1986 he returned to the clinic of MUDr. A. Sosna, CSc., Of whom the then dean of the faculty is prof. Pacovsky promised habilitation without political conditions. After the so-called Velvet Revolution, a number of personnel changes took place at most clinics, which cannot be avoided even by the 1st Orthopedic Clinic, where after the bankruptcy proceedings doc. MUDr. A. Sosna, CSc., Who defends his doctorate after 2 years and is appointed professor. Under his leadership, the traditional programs of the 1st Orthopedic Clinic are being developed, ie alloplasty of the hip, knee, shoulder, elbow and small joints of the wrist and hand, rheumatic surgery, arthroscopic surgery and musculoskeletal traumatology. New types of knee replacements are emerging - WU, SVL and WM, 2 types of shoulder joint endoprostheses - ProSpon, MIL and wrist endoprostheses and CM thumb joint. The development of small metacarpophalangeal and interphalangeal joints is also completed. Due to the difficult space conditions and the deteriorating technical condition of the clinic, the 1st Orthopedic Clinic has been relocated to new premises in the so-called Blue Pavilion of the University Hospital in Motol, where it still works in very good technical conditions. It follows from the above facts that the 1st Orthopedic Clinic has maintained the tradition and spirit of the great founder of modern orthopedics, prof. Gardener. This is also documented by the number of his significant direct and indirect students who received their education at the clinic and especially a certain way of thinking and later became the heads of various clinics and orthopedic departments. |
- Information for patients with plaster bandage
- Hallux valgus
- Hallux rigidus
Plaster bandage care
- Your cast needs 1 to 3 days to dry!
Plaster bandage on the upper limb:
- If you are in bed, place the injured limb on a pillow.
- The hand must always lie higher than the body.
- If you are out of bed, put the injured limb in a sling with the fingers placed above the elbow.
- Move your fingers for a few minutes every half hour.
Plaster bandage on the lower limb:
- In bed, place the injured limb on a pillow.
- The leg must always lie higher than the body.
- If you are sitting, raise the injured limb and place it on a chair higher than the level of the heart.
- Move your toes for a few minutes every half hour.
If the plaster bandage is tight:
- Move your fingers and lift the limb.
- If the feeling of distress does not decrease, see a doctor.
See a doctor immediately for the following conditions:
- Numbness or tingling in the fingers.
- With increasing swelling of the fingers that does not subside within 30 minutes when the position is raised.
- When the fingers turn white or blue.
- In severe pain.
How to use crutches:
- The top of the crutch should be 3 fingers below the armpit.
- The handle of the crutch should reach the wrist when the arm is extended.
- Do not transfer your full weight to your armpits, but support yourself on your hands.
- When walking, place the crutches about 30 cm in front of the legs, lean on the crutches and take a step with the healthy leg.
How to use the stick:
- Carry a cane on your side healthy extremities
How to use a simple arm hanger:
- The sling should support the arm so that the hand is placed higher than the elbow.
- The curtain should also cover and support part of the hand.
Other related instructions:
- Take prescribed medication (for pain and thrombosis).
- Inform your GP as soon as possible.
Hallux valgus
Big thumb (hallux valgus) is an acquired deformity of the foot. It is a complex lesion of the forefoot with a disorder of the thumb. In the Czech Republic, various superstitions and myths are circulating about the operation of the thumb. Some of them are not based on the truth and many of them are based on ways of operational solutions in the past. Currently, modern approaches are used in treatment, which shortens the length of hospitalization and convalescence. These methods significantly changed the possibility of revalgization, ie the re-creation of the arched toe. Due to concerns, patients often postpone surgeries and come to the doctor only when the condition is significantly advanced. In the advanced stages, it is sometimes impossible to save the joint.
Improper thumb position overloads other parts of the foot. Different types of forefoot pain can occur on the basis of the arched toe, which is located in the area of the base of the toe or in the toes.
Conservative therapy
As part of conservative therapy, the use of interdigital concealers and orthopedic insoles for shoes is recommended. Physiotherapy is the most important component of conservative therapy. It improves the position of the foot (holding the arch of the foot), improves the strength of the leg muscles when standing and walking, adjusts the stereotype of walking and the involvement of the thumb in the rebound phase. The use of different types of patch fixations (taping) of the forefoot serves to strengthen the thumb and keep it in a better position when walking.
The significant load on the forefoot even during normal activities means that conservative procedures are often not effective in the treatment of manifestations of hallux valgus deformity. In cases of long-term pain that persist despite the use of conservative therapy, it is appropriate to choose a surgical solution. The operation can be performed under general anesthesia or only under local anesthesia. The time of postoperative recovery depends on the type of operation used and the individual course of healing. After the operation, it is necessary to take into account the impossibility of full load on the operated limb and the need to walk on crutches with a limited step on the operated limb.
Operation
The operation serves to remove the deformity and therefore it is almost always necessary to perform an osteotomy (bone intersection). The first instep bone in the forefoot most often intersects and its correct position is always ensured by screws or staples. These operations can be performed with an open approach or with a more modern closed approach under the control of an X-ray machine. It is these new procedures that shorten the length of recovery after surgery and shorten the time needed to return to a full life.
The operations that are performed at our clinic include operations: Austin, Akin, L chevron (ReveL), SCARF, Lapidus. These types of operations also have their own modifications and are often combined. Our workplace also specializes in the correction of severe deformities after previous operations and destruction in systemic diseases (rheumatoid arthritis, psoriatic arthritis).
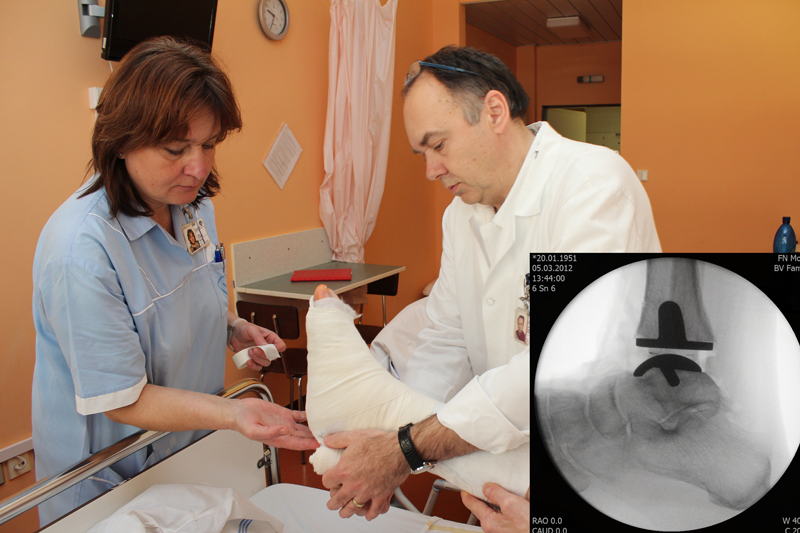
Hallux rigidus
A stiff thumb (hallux rigidus) is an acquired deformity of the foot. It is a degenerative disease of the basic thumb. Osteoarthritis of this joint leads to narrowing of the joint space and loss of cartilage on the articular surfaces. Growths (osteophytes) penetrate at the edges of the joint surfaces, which subsequently prevent the joint from moving. Often, this disease results from a combination of several factors, such as congenital predisposition and frequent minor joint injuries.
Conservative therapy
As part of conservative therapy, the use of orthopedic insoles for shoes and the application of steroidal (anti-inflammatory) injections into the joint is recommended. Conservative procedures are usually ineffective and disease progression.
Operation
Surgery to eliminate the causes and consequences of the disease. The procedures are targeted at the base of the big toe or the first instep bone. It is usually necessary to perform an osteotomy (bone intersection) and always remove bone growths. Operations that are performed at our clinic include, Moberg (proximal toe) osteotomy, Youngswick (first and squeezing of the first femur), arthrodesis (stiffening of the base of the thumb) and joint replacements (entoprosthesis of the basal joint of the big toe).
Surgical treatment can be performed under general anesthesia or only under local anesthesia. The time of postoperative recovery depends on the type of operation used and the individual course of healing. After the operation, it is necessary to take into account the impossibility of full load on the operated limb, which lasts for about 3-6 weeks, and the need to walk on crutches with a limited step on the operated limb.
Master's degree
Orthopedics, 4th year
Orthopedics, 4th year
Optional subjects
Musculoskeletal endoprosthetics 1
Musculoskeletal endoprosthetics 2
Endoprosthesis of the locomotion apparatus 1
Endoprosthesis of the locomotion apparatus 2
Propaedeutics and basics of surgical techniques in musculoskeletal traumatology 1
Propaedeutics and basics of surgical techniques in musculoskeletal traumatology 2
Propaedeutics and basics of surgical techniques in orthopedics 1
Propaedeutics and basics of surgical techniques in orthopedics 2
Clinical seminars
Clinical seminars of the Orthopedic Clinic of the 1st Faculty of Medicine, Charles University and FNM; Autumn 2014
Clinical seminars of the Orthopedic Clinic of the 1st Faculty of Medicine, Charles University and FNM; spring 2015
Information for students of the 4th year of the 1st Faculty of Medicine, Charles University, classified according to the study schedule
to the 1st Orthopedic Clinic of the XNUMXst Medical Faculty of Charles University and the University Hospital Motol
Dear colleagues!
Welcome to our clinic, where Orthopedics and Traumatology of the Musculoskeletal System are taught for 2 weeks, ending with a credit and then an exam.
Basic instructions:
- Students will meet in the morning in the library of the clinic: FN Motol, blue pavilion, ground floor, clinic secretariat between node B and C.
- Classes begin at 8:20 attendance.
- Each day of classes begins with a lecture on the topic from 8:30 to about 10 o'clock.
- Subsequently, students are divided and taken to individual practical workplaces: orthopedic clinics, trauma clinics, operating rooms.
- You will put away your personal belongings before the practical training. Those students who go to the ambulance must have a white coat and a visible student ID; no white coat needed on the operating room.
- On Tuesday of the second week, classes are taking place at the Spondylosurgery Clinic. In agreement with the head of teaching at this clinic, this day you will meet with the teacher at the Motol University Hospital, Blue Pavilion, 2nd floor, node C.
- Practical training will take place until about 12-12: 30 hours, according to the current program of the operating room and ambulance.
- One absence can be excused for 10 days of teaching. In the event of a longer absence, the situation is always resolved individually with the head of teaching, Professor Pokorný (during his absence with Associate Professor Fulín - via e-mail or via the clinic's secretariat).
- During the Covid 19 epidemic, you will be informed by letter, at the e-mail address provided by you in the SIS, before the start of the course, about the current measures. These, of course, result from the measures listed on the website of our Faculty.
- The exams take place in a classic - full-time form - according to the announced dates (dates are announced by the head of the lesson - it is possible to adjust them in advance according to the schedule of afternoon lessons, other exams, etc.). The basis of preparation for questions from Orthopedics is the textbook Basics of Orthopedics. All seminars are available as presentations at MS Teams.
- According to the rules of division of circles into different clinics, only students who have trained at our clinic and are therefore assigned to us according to the schedule can apply for the exam at our clinic.
Dear colleagues, if you have any comments or questions during the teaching at our clinic, do not hesitate to write to me directly to my e-mail address. The goal of us - the teachers - is to make the teaching beneficial and interesting for you.
David Pokorny
Email: david.pokorny@lf1.cuni.cz
Prof. MUDr. David Pokorny, CSc.
Deputy Head of the Teaching Clinic
I. orthopedic clinic of the 1st Medical Faculty of Charles University and University Hospital Motol
Master studies
Teaching Orthopedics for Master's Degree Program and measures associated with pandemic COVID-19
Distance education of orthopedics and traumatology at the 1st Department of Orthopedic, 1st. Faculty of Medicine, Charles University and University Hospital Motol will be primarily provided by professional publications that are already published in SIS system and lectures on the main topics of orthopedics and traumatology. Lectures and webinars will be available in Microsoft Teams application provided by multilicence of our faculty and will be verbally commented in English.
Microsoft Teams link:
Doc. MD Ratsilav Hromadka, Ph.D.
Deputy Head of Teaching for English Parallel, rastislav.hromadka@gmail. com
First week
|
Second week
|
Musculoskeletal endoprosthetics 1, Master's degree
4th year, compulsory-optional, winter semester, always Monday from 14.00 pm
- Details (169,23 KB)
Musculoskeletal endoprosthetics 2, Master's degree
4th year, compulsory-optional, summer semester, always Monday from 14.00 pm
- Details (170,80 KB)
Propaedeutics and basics of surgical techniques in musculoskeletal traumatology 1
3rd - 6th year, compulsory-optional, winter semester
- Details (146,03 KB)
Propaedeutics and basics of surgical techniques in musculoskeletal traumatology 2
3rd - 6th year, compulsory-optional, summer semester
- Details (113,63 KB)
Propaedeutics and basics of surgical techniques in orthopedics 1
3rd - 6th year, compulsory-optional, winter semester
- Details (112,25 KB)
Propaedeutics and basics of surgical techniques in orthopedics 2
3rd - 6th year, compulsory-optional, summer semester
- Details (112,50 KB)
Endoprosthesis of the locomotion apparatus 1, master study
4th year, obligatory elective subject, Winter term, every Monday starting at 2PM
- Details (204,60 KB)
Endoprosthesis of the locomotion apparatus 2, Master study
4th year, obligatory elective subject, Summer term, every Monday starting at 2PM
- Details (164,63 KB)
Ambulance files
Orthopedic file, tel .: (224) 433 925
Traumatology file, tel .: (224) 438 624
Ambulance
1st ambulance, tel .: (224) 433 973
2st ambulance, tel .: (224) 433 974
3st ambulance, tel .: (224) 433 975
4st ambulance, tel .: (224) 433 976
5st ambulance, tel .: (224) 433 978
6. Ambulance, phone: (224) 433 930
7st ambulance, tel .: (224) 433 977
Traumatology ambulance, tel. (224) 438 662
Inpatient stations
1st station, tel .: (224) 433 933
2st station, tel .: (224) 433 934
3st station, tel .: (224) 433 935
4th station (trauma department), tel .: (224) 438 630
Septic department, tel .: (224) 433 989
Orthopedic ICU, tel .: (224) 433 940
Traumatological ICU, tel .: (224) 438 638
Operating rooms
Orthopedic operating rooms, tel .: (224) 438 407
Emergency operating theaters, tel .: (224) 438 422