- Basic information
- Management and staff
- Specialization
- For the professional public
- Teaching
- Publications
- Books
- Information for patients
- How to order from us?
- The course of my hospitalization
- Postoperative rehabilitation
- Baggage to the hospital
- Glossary of backbone terms
- Verticalization from the bed
- History
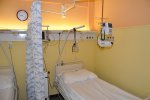
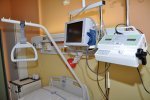
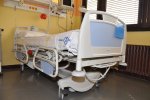
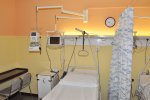
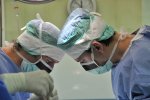
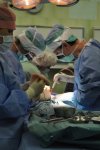
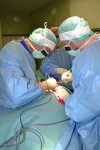
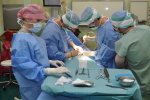
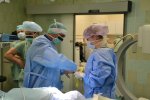
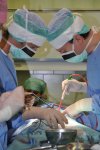
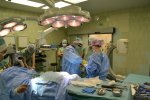
- Gallery
- Contact

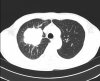
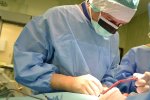
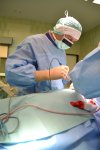
The Department of Spondylosurgery of the 1st Medical Faculty of Charles University and the Motol University Hospital is a specialized workplace dealing with spine surgery. The Department of Spondylosurgery of the 1st Medical Faculty of Charles University and the Motol University Hospital are among the leading centers in the Czech Republic in terms of the number of procedures performed and the scope of care provided.
The subject of her interest are practically all diseases of the spine: spinal cord injuries, degenerative diseases, cancer, spinal inflammations, congenital deformities.
The clinic makes full use of the unique possibilities of the Motol hospital, interdisciplinary cooperation of all experts in the care of patients with spinal diseases, starting with modern diagnostic methods and ending with specialized care for patients with spinal cord injuries.
The clinic provides care for injuries and emergencies 24 hours a day through a counseling system. He also performs continuous superconsulting activities for a number of district and smaller hospitals.
At our clinic, we perform almost every year 1400 spine surgery, around 12 000 patients is treated on an outpatient basis and 1600 patients hospitalized.

Prof. MUDr. Jan Stulik CSc.
Secretariat
(224) 432 581
Head of the clinic
Prof. MD Jan Štulík, CSc.
Tel .: 224432580, 2581
Email: jan.stulik@fnmotol.cz

Deputy head for medical and preventive activities
as. MD Jan Kryl
Tel .: 224432580, 2581
Email: jan.kryl@fnmotol.cz
Chief doctors
Standard department
as. MUDr. Tomas Vyskocil
Tel .: 224432573, 2572
Email: tomas.vyskocil@fnmotol.cz
Jip
as. MD Michal Barna
Tel .: 224432589, 2590
Email: michal.barna@fnmotol.cz
Doctors of spondylosurgery clinic
prof. MUDr. Zdenek Klezl, CSc.
Tel .: 224432574, 2599
MD Gábor Geri
Tel .: 224432589, 2590
MD Filip Pivarči
Tel .: 224432589, 2590
MD Lucie Salavcová
Tel .: 224432573, 2599
MD Michaela Rybárová
Tel .: 224432573, 2599
MD Michal Varga
Tel .: 224432573, 2599
MD Richard Hajduk
Tel .: 224432573, 2599
MD Jan Zemanek
Tel .: 224432573, 2599
MD Eva Vaskova
Neurologist, Center for Conservative Therapy (CKT FNM)
Phone: 224432575
Head nurse
Bc. Lenka Šipulová
Phone: No. 224 432 585
Email: lenka.sipulova@fnmotol.cz
Station ICU
Bc. Markéta Šimová
Tel: 224 432 2590
Email: marketa.simova@fnmotol.cz
Station nurse standard
Irena Kroupová
Phone: 224 432 570, 2573
Email: irena.kroupova@fnmotol.cz
Ambulance station nurse
Eliška Akachi
Tel: 224 432 592
Email: eliska.akachi@fnmotol.cz
The clinic specializes in surgical care for patients with spinal diseases.
Its basic task is a surgical solution spine injury with the subsequent primary phase of rehabilitation of these patients. They also fall into this area conditions after spinal injuries such as kyphotization or stabilization failure. Especially with emphasis on traumatology of the cervical spine, including injuries of the cervico-cranial junction. At present, the task of the department is also the follow-up care of patients with spinal cord injuries until the time of transfer to the rehabilitation workplace - Spinal Unit of the Motol University Hospital.
The clinic also takes care of patients with spinal cancer. This is the primary cancer illnesses and in particular o metastatic disabilities and pathological fractures with oppression of nerve structures, mostly accompanied by neurological deficits.
Another diseases belonging to the spectrum of care of spondylosurgery clinics are inflammation of the spine. They are also an integral part of spinal surgery degenerative diseases spondylosis, spondylarthrosis with cervical and lumbar spine stenosis, degenerative scoliosis, spondylolisthesis, instability. An important part is the surgical treatment of degenerative changes in the cervical spine in rheumatoid arthritis and congenital malformations.
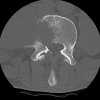
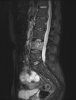
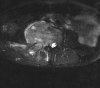
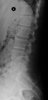
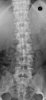
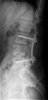
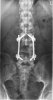
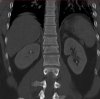
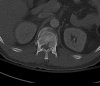
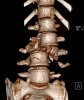
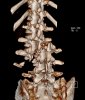
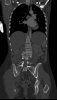
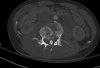
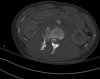
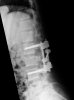
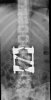
An example of surgical treatment of lumbar spine cancer.
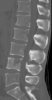
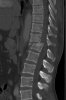
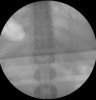
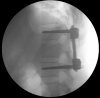
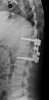
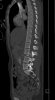
Example of surgical treatment of thoracic spine injuries. Patient with a dislocated fracture of the 12th thoracic vertebra (fr. T12) after falling from above. Primarily posterior position correction with removal of oppression of nerve structures, fixation with an internal transpedicular fixator to the vertebrae above and below the injured floor, including removal of bone grafts from the hip shovel and application of these grafts around the internal fixator (Socon Ti T11-L1, posterior desgraft grafts). Subsequently, in the second period, the replacement of the intervertebral disc between the 11th and 12th thoracic vertebra (T11-T12 discectomy) with a bone graft from the scapula of the hip bone.
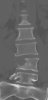
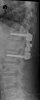
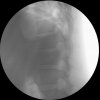
An example of surgical treatment of lumbar spine injuries. A patient with a severe, fragmentary fracture of the 3rd lumbar vertebra struck by a car. Surgical therapy in two periods, primarily posterior correction and fixation with a transpedicular internal fixator with removal of the oppression of nerve structures, followed by anterior replacement of the L3 body with an expandable implant after a few days.
- Teaching
- Publications
- Books
The department teaches students of the 6th year of the 1st Medical Faculty, Charles University in Prague within the internship block at the 3rd Surgical Clinic of the 1st Medical Faculty of Charles University. The aim of the two-day internship (always on Monday and Tuesday according to the schedule of individual circles) is to acquaint general medicine students in the field of orthopedics and surgery with the issue of spinal diseases, especially with a focus on traumatology. The anatomy of the spine will be repeated in the introduction, as well as the etiology and cause of the disease or injuries. Diagnostics with a focus on classification, in the case of accidents, especially on the most commonly used AO classification today. Last but not least, surgical therapy will be mentioned, but conservative procedures will not be left out. In addition, a mention of regimen measures, dispensary care and prognosis after spinal surgeries.
Furthermore, the department provides training for bachelors and masters of nursing at the 2nd Medical Faculty of Charles University and internships within the subject of nursing for students of the 2nd year of the 2nd Medical Faculty, Charles University in Prague. Students practice and improve their practical skills under the supervision of a competent nurse. As part of the provision of nursing care, they are led to apply the method of the nursing process. The seminars, which are organized by cheating the head nurse with the cooperation of station nurses, are aimed at deepening theoretical knowledge about nursing activities.
1. KRBEC, M., ŠTULÍK, J .: „Pincer "fractures of the thoracolumbar spine. Acta Chir.
orthop. Dream. Czech, 64/6: 337-341, 1997.
2. STEHLIK, J., STULIK, J .: The actual method of treatment of dislocated heel fractures
bones. Rozhl. Chir. 77/9: 389-395, 1998.
3. KRBEC, M., STULIK, J .: Extension fractures of the thoracolumbar spine. Acta Chir.
orthop. Dream. Czech, 65/5: 292-295, 1998.
4. DOUBKOVÁ, A., KRBEC, M., ŠTULÍK, J., ŠTĚŇHOVÁ, H .: Topography of structures
placed in front of the thoracic and lumbar spine. Acta Chir. orthop. Dream. Czech, 66/4:
206-212, 1999.
5. ŠTULÍK, J., KRBEC, M .: Os odontoideum- posttraumatic instability C1-2. Record
Chir. orthop. and dream. Czech, 66/6: 356-361, 1999.
6. KRBEC, M., STULIK, J .: Pararectal miniinvasive retroperitoneal approach
to the lumbosacral transition. Acta Chir. orthop. and dream. Czech, 67/1:
13-16, 2000.
7. ŠTULÍK, J., KRBEC, M .: Magerl fixation technique C1-2. Acta Chir. orthop.
Dream. Czech, 67/2: 93-99, 2000.
8. KRBEC, M., ŠTULÍK, J .: Treatment fractures of the Th-L spine by an internal fixator.
Evaluation of 120 operated cases. Acta Chir. orthop. Dream.
Czech, 68/2: 77-84, 2001.
9. BARTONÍČEK, J., JEHLIČKA, D., ŠTULÍK, J .: Tensile cerclage with screws -
forgotten technique? Acta Chir. orthop. Dream. Czech, 68/3: 188-191, 2001.
10. ŠTULÍK, J., KRBEC, M .: Atlantoaxial rotational dislocation (case report). Acta Chir.
orthop. Dream. Czech, 69/1: 49-53, 2002.
11. KOPSKÝ, V., VEČEŘOVÁ, J., MELČÁK, I., PLISS, A., ŠTULÍK, J., RAŠKA, I .:
ATP dependent step is required for the translocation of microinjected precursor
mRNA into nuclear speckles. Folia Biologica (Prague), 48: 69-72, 2002.
(IF 0,351)
12. ŠTULÍK, J., KRBEC, M., HAVRÁNEK, P .: Boundary indications for Magerl fixation
C1-C2 (case study). Acta Chir. orthop. Dream. Czech, 69/2, 108-112, 2002.
13. ŠTULÍK, J., SUCHOMEL, P., LUKÁŠ, R., CHROBOK, J., KLÉZL, Z.,
TALLER, S., KRBEC, M .: Direct dental osteosynthesis - a multicenter study. Record
Chir. orthop. Dream. Czech, 69/3, 141-148, 2002.
14. KRBEC, M., ŠTULÍK, J., TICHÝ, V .: Vertebral body replacement with expansion
implant (Synex). Acta Chir. orthop. Dream. Czech, 69/3, 158-162, 2002.
15. STOKROVÁ, J., KORB, J., PLISS, A., RAŠKA, I., ŠTULÍK, J., DVOŘÁKOVÁ, M .:
Overexpression of v-myb oncogene or c-myb proto-oncogene in insect cells:
Characterization of newly induced nucleolus.like structures accumulating Myb
protein. Int. J. Mol. Med., 9/5: 547-554, 2002. (IF 1,899)
16. STEHLIK, J., STULIK, J.: Combined method of treatment of heel fractures.
Acta Chir. orthop. Dream. Czech, 69/4: 209-218, 2002.
17. ŠTULÍK, J., KRBEC, M., VYSKOČIL, T .: Use of bioceramics in treatment
fractures of the TL spine. Acta Chir. orthop. Dream. Czech, 69/5: 288-294, 2002.
18. MALINSKÝ, J., KOBERNA, K., BEDNÁŘ, J., ŠTULÍK, J., RAŠKA, I .: Searching
for active ribosomal genes in situ: light microscopy in light of the electron beam.
J. Structural Biology, 140/3, 227-231, 2002. (IF 3,671)
19. ŠTULÍK, J., KRBEC, M., VYSKOČIL, T .: Injury of lower cervical spine -
CSLP monocortical system. Acta Chir. orthop. Dream. Czech, 70/4: 226-
232, 2003.
20. ŠTULÍK, J., KRBEC, M .: Atlas fractures. Acta Chir. orthop. Dream. guild.,
70/5, 274-278, 2003.
21. SUCHOMEL, P., ŠTULÍK, J., KLÉZL, Z., CHROBOK, J., LUKÁŠ, R., KRBEC,
M., MAGERL. F: Transarticular fixation C1-C2: multicenter retrospective
study. Acta Chir. orthop. Dream. Czech, 71: 6-12, 2004.
22. ŠTULÍK, J., VYSKOČIL, T., ŠEBESTA, P., KRYL, J: Harms fixation technique
C1-C2. Acta Chir. orthop. Dream. Czech, 72/1: 22-27, 2005.
23. JANIK, V., DANIEL, J., PADR, R., NEUWIRTH, J., VYSKOCIL, T., KRYL, J.,
ŠEBESTA, P., ŠTULÍK, J .: Percutaneous vertebroplasty using 3D rotation
seriography. Czech. Radiol, 59: 171-177, 2005.
24. ŠTULÍK, J., VYSKOČIL, T., ŠEBESTA, P., KRYL, J: Complex atlantoaxial
fractures. Acta Chir. orthop. Dream. Czech, 72/2: 105-110, 2005.
25. ŠTULÍK, J .: Injuries to the middle cervical spine and cervicothoracic junction.
Neurology for Practice, 6: 78-81, 2005.
26. ŠTULÍK, J., VYSKOČIL, T., ŠEBESTA, P., KRYL, J., PAFKO, P .: Surgical treatment
diseases of the cervicothoracic junction. Acta Chir. orthop. Dream. guild.,
72/4: 213-220, 2005.
27. ŠEBESTA, P., ŠTULÍK, J., KRYL, J., VYSKOČIL, T: Unilateral chest dislocation
and lumbar spine. Acta Chir. orthop. Dream. Czech, 72/5: 317-321, 2005
28. ŠEBESTA, P., ŠTULÍK, J., KRYL, J., VYSKOČIL, T: Purulent arthritis
intervertebral joint. Acta Chir. orthop. Dream. Czech, 72/6: 387-389, 2005.
29. ŠTULÍK, J., VYSKOČIL, T., BODLÁK, P., ŠEBESTA, P., KRYL, J., VOJÁČEK,
J., PAFKO, P .: Injuries to large vessels during anterior access to the thoracic and lumbar
spine. Acta Chir. orthop. Dream. Czech, 73/2: 92-98, 2006.
30. ŠTULÍK, J., PEŠL, T., KRYL, J., VYSKOČIL, T., ŠEBESTA, P., HAVRÁNEK, P .:
Spinal injuries in children and adolescents. Acta Chir. orthop. Dream. Czech Republic, 73/5:
313-320, 2006
31. KRYL, J., ŠTULÍK, J., VYSKOČIL, T., ŠEBESTA, P .: Spinal injuries
nail. Acta Chir. orthop. Dream. Czech, 73/5: 353-355, 2006.
32. SYKOVÁ, E., HOMOLA, A., MAZANEC, R., LACHMANN, H., LANGKRAMER
KONRÁDOVÁ, Š., KOBYLKA, P., PÁDR, R., NEUWIRTH, J., KOMRSKA, V.,
VÁVRA, V., ŠTULÍK, J., BOJAR, M .: Autologous bone marrow transplantation in
patients with subacute and chronic spinal cord injury. Cell Transplantation, 15:
1-13, 2006. (IF 3,481)
33. STULIK, J., STEHLIK, J., RYSAVY, M., WOZNIAK, A .: Minimally-invasive
treatment of intra-articular fractures of the cancaneum. J. Bone Jt Surg., 88-B:
1634-1641, 2006. (IF 1,790)
34. PAVELKA, T., DŽUPA, V., ŠTULÍK, J., GRILL, R., SKÁLA-ROSENBAUM, J .:
Results of surgical treatment of unstable pelvic ring injuries. Acta Chir.
orthop. Dream. Czech, 74/1: 19-28, 2007.
35. ŠTULÍK, J., KOZÁK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J.,
PELICHOVSKÁ, M .: Total spondylectomy of C2: a new surgical technique. Record
Chir. orthop. Dream. Czech, 74/2: 79-90, 2007.
36. ŠTULÍK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J .: Atlantoaxial fixation using
the polyaxial screw-rod system. Eur Spine J, 16: 479-484, 2007. (IF 1,824)
37. ŠTULÍK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J .: Cervical spine injuries in
patients over 65 years of age. Acta Chir. orthop. Dream. Czech, 74/3: 189-194, 2007.
38. KLÉZL, Z., ŠTULÍK, J., KRYL J., ŠEBESTA, P., VYSKOČIL, T., BOMMIREDDY,
R., CALTHORPE, D .: Surgical treatment of spinal infectious disease. Acta Chir.
orthop. Dream. Czech, 74/5: 305-317, 2007.
39. STULIK, J., PITZEN, TR, CHROBOK, J., RUFFING, S., DRUMM, J., SOVA,
L., KUCERA, R., VYSKOCIL, T., STEUDEL, W. I: Fusion and Failure following
Anterior Cervical Plating with Dynamic or Rigid Plates: 6 month Results of a
Multicentric, Prospective, Randomized, Controlled Study. Eur Spine J, 16: 1689-
1694, 2007. (IF 1,824)
40. ŠTULÍK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J .: Dent fractures u
patients over 65 years of age: direct dental osteosynthesis vs. rear fixation C1-C2. Record
Chir. orthop. Dream. Czech, 75/2: 99-105, 2008.
41. ŠEBESTA, P., ŠTULÍK, J., VYSKOČIL, T., KRYL, J .: Zad stabilization of fragmentation
L5 fractures without anterior column treatment. Acta Chir. orthop. Dream. guild.,
75/2: 123-128, 2008.
42. PYCHA, K., RYGL, M., BLAŽEK, D., KEIL, R., ŠTULÍK, J., ŠNAJDAUF, J .: Total
prepyloric transection of sewers and vertebral trauma: case report and review of
the literature. Pediatrician. Surg. Int., 2008. (IF 0,653)
43. HEJČL, A., LESNÝ, P., PŘÁDNÝ, M., MICHÁLEK, J., JENDELOVÁ, P.,
ŠTULÍK, J., SYKOVÁ, E .: Biocompatible hydrogels in spinal cord injury repair.
Physiol. Res., 2008. (IF 1,505)
44. ŠTULÍK, J., KRYL, J., NESNÍDAL, P .: History of treatment of cervical spine injuries and
spinal cord. Orthopedics, 2: 184-190, 2008.
45. STULIK, J., BARNA, M., NESNÍDAL, P .: Middle cervical spine injury a
cervicothoracic junction. Orthopedics, 2: 160-166, 2008.
46. ŠTULÍK, J., KRYL, J., VYSKOČIL, T., ŠEBESTA, P., KRBEC, M., TRČ, T .:
Prodisc C mobile intervertebral disc replacement - prospective
monocentric two-year study. Acta Chir. orthop. Dream. Czech, 75/4: 253-261,
2008.
47. PITZEN, T., CHROBOK, J., STULIK, J., RUFFING S., DRUMM, J., SOVA, L.,
KUČERA, R., VYSKOČIL, T., STEUDEL, WI: : Implant complications, Fusion,
loss of lordosis, and outcome following anterior cervical plating with
dynamic or rigid plates: 2 years results of a multi-centric, randomized, controlled
study. Spine, 34: 641-646, 2009. (IF 2,351)
48. ŠRÁMEK, J., ŠTULÍK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J., NESNIDAL,
P., BARNA, M .:Hyperextensive injury of the cervical spine in spondylosis. Acta Chir.
orthop. Dream. Czech, 76: 128-132, 2009. (IF 1,628)
49. BUREŠOVÁ, M., KEIL, R., HRDLIČKA, L., ŠŤOVÍČEK, J., ŠTULÍK, J .:
Spondylodiscitis mimicking esophageal tumor. Endoscopy, 18: 175-177, 2009.
50. ŠTULÍK, J., KLÉZL, Z., ŠEBESTA, P., KRYL J., VYSKOČIL, T .:
Occipitocervical fixation: long-term follow-up of 57 patients. Acta Chir. orthop.
Dream. Czech Republic, 76: 479-486, 2009. (IF 1,628)
51. ŠEBESTA, P., ŠTULÍK, J., VYSKOČIL, T., KRYL, J .: Kaudy's syndrome
elective power on the lumbar spine. Acta Chir. orthop. Dream. Czech, 76: 505-
508, 2009. (IF 1,628)
52. NESNÍDAL, P., ŠTULÍK, J., ŠEBESTA, P .: Pulmonary embolization
polymethyl methacrylate-a rare complication of percutaneous vertebroplasty. Acta Chir.
orthop. Dream. Czech, 77: 337-340, 2010.
53. KOLÁŘ, P., ŠTULÍK, J., KYNČL, M .: Dynamic examination of the lumbar spine
using magnetic resonance imaging. Cesk Slov Neurol N, 73/106: 438-442,
2010. (IF 0,393)
54. ŠTULÍK, J., KOZÁK, J., ŠEBESTA, P., VYSKOČIL, T., KRYL, J., KLÉZL, Z .:
Total spondylectomy of C2: report of three cases and review of the literature.
J Spinal Disord Tech, 23 (8): e53-58, 2010. (IF 1,206)
55. ŠTULÍK, J., NESNÍDAL, P., ŠEBESTA, P., VYSKOČIL, T., KRYL, J .: Kyphotic
cervical spine deformities. Acta Chir. orthop. Dream. Czech, 78: 215-224, 2011.
56. JAKUBÍKOVÁ, M., PŘÍHODOVÁ, I., BARNA, M., ŠTULÍK, J., VANĚK, P.,
BENEŠ, V., NEVŠÍMALOVÁ, S .: Spinal complications in genetic syndromes
case studies. Cesk Slov Neurol N, 74/107: 482-485, 2011. (IF 0,393)
57. STULIK, J., BARNA, M., KRYL, J .: Surgical treatment of atlantoaxial osteoarthritis
(AAOA): a prospective study of 27 patients. Acta Chir. orthop. Dream. Czech, 79:
31-36, 2012.
58. NESNÍDAL, P., ŠTULÍK, J., BARNA, M .: Spinal cord commotion: a retrospective study 24
patients. Acta Chir. orthop. Dream. Czech, 79: 150-155, 2012.
59. BARNA, M., ŠTULÍK, J., FENCL, F .: Metatropic dysplasia as a cause
atlantoaxial instability, spinal canal stenosis and myelopathy: case report a
literature review. Acta Chir. orthop. Dream. Czech, 79: 169-174, 2012.
60. BARNA, M., ŠTULÍK, J., KRYL, J., VYSKOČIL, T., NESNÍDAL, P .: Mobile
cervical intervertebral disc replacement ProDisc-C: prospective monocentric
four-year study. Acta Chir. orthop. Dream. Czech, 79: 512-519, 2012.
61. ŠTULÍK, J., NESNÍDAL, P., KRYL, J., VYSKOČIL, T., BARNA, M .: Unstable
upper cervical spine injuries in children and adolescents. Acta Chir. orthop. Dream.
Czech, 80: 106-113, 2013. (IF 0,416)
62. VANÚČEK, V., KLIMA, K., KOHOUT, A., FOLTÁN, R., JIROUSEK, O., SEDÍ, J.,
STULÍK, J., SYKOVÁ, E., JENDELOVA, P.: The combination of mesenchymal
stem cells and a bone scaffold in the treatment of vertebral body defects. EUR
Spine J, 22 (12): 2777-2786, 2013. (IF 2,130)
63. KLEZL, Z., SWAMY GN, VYSKOCIL, T., KRYL, J., STULIK, J .: Incidence of
vascular complications arising from anterior spinal surgery in the thoraco-lumbar
spine. Asian Spine J, 8: 59-63, 2014. (IF 0,158)
64. ŠTULÍK, J., ADÁMEK, S., BARNA, M., KASPŘÍKOVÁ, N., POLANECKÝ, O.,
KRYL, J .: Axial Lumbar Intervertebral Fusion-AxiaLIF: Prospective
monocentric study. . Acta Chir. orthop. Dream. Czech, 81: 203-211, 2014.
(IF 0,416)
65. SUCHOMEL, P., JURÁK, L., ANTINHEIMO, J., POJHOLA, J., STULIK, J.,
MEISEL, HJ, CABRAJA, M., WOICIECHOWSKY, C., BRUCHMANN, B.,
SHACKLEFORD, I., ARREGUI, R., SOLA, S .: Does saggital position of the
CTDR-related center of rotation influence functional outcome? Prospective 2-
annual follow-up analysis. Eur Spine J, 23/5: 1024-1034, 2014. (IF 2,130)
66. LUKÁŠ, R., ŠTULÍK, J., ŠRÁM, J., PAZOUR, J., KŘÍŽ, J., NESNÍDAL, P .:
Suboptimal surgical treatment of spine fractures with neurological impairment.
Cesk Slov Neurol N, 77/107: 734-740, 2014. (IF 0,393)
67. KLIMA, K., VANÚČEK, V., KOHOUT, A., JIROUSEK, O., FOLTÁN, R., STULÍK, J., SEDÍ, J., MACHOŇ, V., PAVLÍKOVÁ, G.., JENDELOVA, P., SYKOVÁ, E., SEDÝ, J.: Stem cells regenerative properties on new rat spinal fusion model. Physiol Res. 2014. (IF 1,487)
68. ŠTULÍK, J., NESNÍDAL, P., KRYL, J., VYSKOČIL, T., BARNA, M., KLÉZL, Z .:
Total en bloc spondylectomy of C3: A new surgical technique and literature
review. Acta Chir. orthop. Dream. Czech, 82: 261-267, 2015. (IF 0,416)
69. BARNA, M., ŠTULÍK, J., KRYL, J., VYSKOČIL, T., NESNÍDAL, P .: Collet-
Sicard's syndrome in occipital condyle fracture. Acta Chir. orthop. Dream.
Czech, in press.
70. NESNÍDAL, P., ŠTULÍK, J., LISCHKE, R., BARNA, M .: Bulky gaglioneur
spine and mediastinum. Acta Chir. orthop. Dream. Czech, waiting
1. STEHLIK, J., ŠTULÍK, J .: Heel bone fractures. Prague, Galen 2005.
2. STEHLIK, J., ŠTULÍK, J .: Calcaneal fractures. . Prague, Galén 2010.
3. ŠTULÍK, J. et al .: Cervical spine injuries. Prague, Galen 2010.
4. ŠTULÍK, J. et al .: Cervical spine trauma. Prague. Galén 2012.
1. ŠTULÍK, J .: Surgical treatment of spinal diseases. In: KOLÁŘ, P. et al .:
Rehabilitation in clinical practice. Prague, Galen 2010.
2. KLÉZL, Z., SWAMY, G., N., STULIK, J .: The rheumatoid cervical spine. In:
BENTLEY, G .: EFORT istructional lectures book. Volume 10, Dordrecht,
Heidelberg, London, New York, Springer, 2010.
3. ŠTULÍK, J .: Spinal injuries in children and adolescents. In: HAVRÁNEK, P. et al .:
Child fractures. Prague, Galen 2013.
4. ŠTULÍK, J .: Spinal injuries. In: ZEMAN, M., KRŠKA, Z. et al .: Special
surgery, Galen, 2014.
5. ŠTULÍK, J .: Spinal injuries. In: DUNGL, P. et al .: Orthopedics, City, 2014
6. STULÍK, J .: Surgical treatment of spinal diseases. In: KOLÁŘ, P. et al .: Clinical
rehabilitation. Prague, Galen 2012.
7. KLÉZL, Z., STULIK, J .: Surgical treatment of the cervical spine in rheumatoid
arthritis. In: BENTLEY, G .: European surgical orthopedics and traumatology, The
EFORT textbook. Volume 2, Heidelberg, New York, Dordrecht, London, Springer,
2014.
8. KLÉZL, Z., BHANGOO, NS, STULIK, J .: Treatment of cervical facet
subluxations, dislocations and fracture-dislocations. In: BENTLEY, G .: EFORT
instructional lecture book. Volume 15, Dordrecht, Heidelberg, London, New York,
Springer, 2015.
| From November 9, 11, the spondylosurgery outpatient clinic, including the Conservative Therapy Center, has been moved to the lower ground floor – P floor, node E. |
Information for patients
How to order from us?
Order only by phone: 224 432 592
| Monday | morning 7:30 - 11:30 a.m | |
| Tuesday - Friday | morning 7:30 - 9:00 a.m | afternoon 11:30 p.m. - 13:00 p.m |
Patients with chronic problems
After a phone call, you will only be booked for a day, not for an hour, and to a specific doctor (see below). You can only order on the recommendation of your local doctor or specialist. Bring this recommendation with you on your first visit, especially if you are not from Prague and its surroundings. If you have already completed an examination with imaging methods such as an X-ray, CT or MRI examination, bring their results on a CD carrier. This will significantly speed up the process of deciding on possible surgical therapy for the patient.
Patients in acute conditions
Through the Emergency Department of Motol Hospital, these are spinal injuries without neurological deficit, cancer with progression of neurological symptomatology, degenerative disease with the development of syn. cauda, inflammation of the spine with the development of neurological symptomatology or failure of ATB therapy with the progression of clinical problems.
Who will take care of you?
First of all, our outpatient nurses and then the doctors of our clinic. Outpatient doctors are appointed on the day of the outpatient clinic, so you cannot make an appointment with a specific doctor in advance.
Dear Madam, dear Sir,
you will arrive at our clinic on the day of admission, 6th floor / node B, FN Motol, adult part, best between 9-10 o'clock in the morning to the admissions office. It is located just after entering the department on the left. Here, the administrative staff of our secretariat will handle the most important formalities with you (verification of identity and personal data, health insurance and their entry into the hospital system). Subsequently, you will be admitted by a pre-designated doctor at the ward - they will take a medical history, perform a clinical examination focusing on the examination of the spine, check and prepare the results of imaging examinations, e.g. fills in the missing. The doctor will further instruct you about the nature of the disease and the possibilities of therapy with a focus on the method and course of the operation. They will also explain the complications that may occur during surgery and hospitalization. If you agree with the proposed procedure, you will sign the necessary informed consents (with hospitalization, surgery and administration of blood derivatives). Furthermore, you will be received by a nurse / brother, who will then place you in a predetermined bed. Standard rooms are triple, equipped with private toilet and shower, LCD TV. They are in the standard department of the clinic 2 single superior rooms, in which we provide above-standard accommodation, the room price is 1500 CZK/night. More at the FN Motol stands.
On the day of your admission, there may be a delay between the admission itself and the bedtime, which is due to the necessary administration associated with admitting new and dismissing existing patients. In the afternoon, the anesthesiologist checks it and prepares it before general anesthesia the following day. Patient order the primary department or his deputy always determines the operation for the operation. The order may vary, with preference given to patients with acute spinal disease who have been admitted during the service. Therefore, your planned operation may be postponed or even canceled. We ask for leniency and tolerance with patients who have entered our ward in an acute condition.
Immediately after surgery you will be saved on intensive care unit (node C, 2nd floor), where you will be intensively monitored according to the severity of the operation and your clinical condition. You will also be given effective analgesic therapy, chronic medicines, medicines to prevent deep vein thrombosis and other symptomatic therapies. The length of hospitalization in the intensive care bed is usually 1-3 days with an uncomplicated postoperative course. On the 1st postoperative day, if your condition allows, we will perform a follow-up imaging examination. 2. postoperatively, you will be instructed by the physiotherapist about the movement regime and gradually verticalized with his assistance.
After stabilization of your condition, a translation on a standard bed follows. The practice of verticalization and mobilization, self-service, continues. We will gradually reduce analgesic therapy so that you can be released home without its significant support. The average length of hospitalization in our ward is six days.
If you have any during hospitalization any questions or doubts, don't be afraid to ask your doctor during visits that take place every morning.
Rehabilitation after thoracic and lumbar spine surgery
Dear patient, you have undergone spine surgery at the Department of Spondylosurgery, University Hospital in Motol. We would like to provide you with recommendations on how to behave in the home environment after thoracic or lumbar spine surgery. You should be aware that your spine is still ill and that only the cause of the pain, which is the result of more wear and tear on the spine as a whole, has been removed by surgery. Therefore, it is necessary to recommend how you should treat the diseased spine. These recommendations are also indicated for patients after thoracic or lumbar spine surgery after an injury without a neurological deficit.
Dear patient,
you have undergone spine surgery at the Department of Spondylosurgery, University Hospital in Motol. We would like to provide you with recommendations on how to behave in the home environment after thoracic or lumbar spine surgery.
You should be aware that your spine is still ill and that only the cause of the pain, which is the result of more wear and tear on the spine as a whole, has been removed by surgery. Therefore, it is necessary to recommend how you should treat the diseased spine.
These recommendations are also indicated for patients after thoracic or lumbar spine surgery after an injury without a neurological deficit.
1. On the way home, the nurses will provide you with an ambulance according to the doctor's indication, the transport will take place lying down.
Upon arrival at home, if possible, we recommend staying mostly in bed. The ambulance journey is a sufficient burden for this day.
2. In a home environment, it is advisable to sleep on a flat, raised bed so that you can get up as best you can.
3. Initially, it is advisable to climb the stairs only when accompanied by another person, as a situation may arise in which someone will need to provide you with support.
4. You can put the crutches down briefly while sitting in the toilet. You can start sitting only after the first check-up with a spondylosurgeon, which is usually six weeks after the operation. However, a longer session and complete postponement of the crutches is indicated by the doctor up to three months after the operation.
If you already get permission to sit down, you should start carefully, only for a short time, for example to eat. You should always sit with your back straight. However, you must avoid sitting in a car or a chair for a long time.
Depending on your general health, you can prolong walking outdoors.
5. It is good to practice learned exercises several times a day. Temporarily skip painful exercises.
6. You should avoid movements that are related to the surroundings of the operation site, such as bows, bends, tilts, and rotations. These movements may begin to train slowly up to three months after surgery.
7. We recommend not doing hard physical work, not lifting heavy objects. If necessary, you can get up from a squat and a straight back. Sudden uncoordinated movements, such as slipping, should be avoided. Be careful when walking on uneven terrain.
8. You can shower around the surgical wound after removing the stitches, then it is advisable to dry the wounds with touches and finally lubricate them with a greasy cream.
Bathing in hot water after surgery is not recommended.
9. Rehabilitation is usually indicated at the FNM Department of Spondylosurgery up to three months after surgery.
10. Driving a car while sitting is contraindicated, that is, it is prohibited.
11. Sexual activity is possible if it is not accompanied by pain from the operating field. It is therefore necessary to choose a position in which the spine is relieved, also for a period of three months.
12. We do not recommend sports until six weeks after the operation, the only thing that can be recommended is passive exercise. This is an exercise that allows you to maintain full range of motion in the joints and flexibility of muscles and tendons.
13. After three months, you can slowly start sports such as swimming or cycling.
14. You are entitled to spa treatment within 1 year after the operation. It is advisable to undergo spa treatment about half a year after the operation.
Scar care
The goal of scar care is to heal well and to ensure that the scar moves against the subcutaneous tissue and other structures. It occurs when there are no more scabs on the scar and the skin is completely healed. Let the scar heal, do not tear the scabs around it. Shower the scar for you with a pleasant stream of lukewarm water, but in the first weeks do not soap it, just rinse with water. Keep the scar clean, dry it carefully after bathing and apply a greasy unscented cream to it - this will ensure its suppleness. Apply a so-called pressure massage to the scar (see below). The scar must not be red, hot, purulent and must not bleed.
Exercise unit after lumbar spine surgery
We follow these principles during the exercise:
- We practice slowly
- We perform exercises slowly with a pull, not a swing
- Exercises must not cause pain, if so, we will skip these exercises
- We take 10-second breaks between each exercise
- We breathe regularly during exercise, we do not hold our breath
- We repeat each exercise 5 times, gradually increasing the number of repetitions
- We exercise regularly several times a day
Explanatory notes:
HK ........ one upper limb DK ....... lower limb
HKK ..... both upper limbs HD .... both lower limbs
Walking up the stairs with armpits:
to the stairs: from the stairs
1. First DK 1. Both crutches at once
2. Second DK 2. First DK
3. Both crutches at once 3. Second DK

ZP: crease HD, then with a breath pull the buttocks and abdomen, endurance 5 seconds, relax:
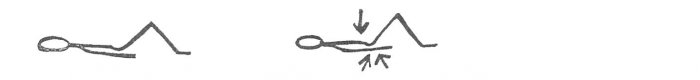
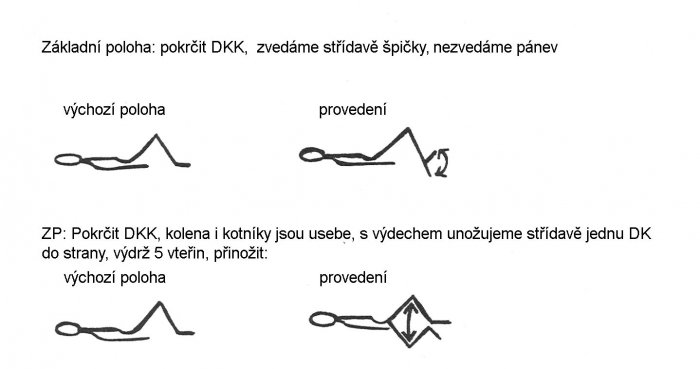
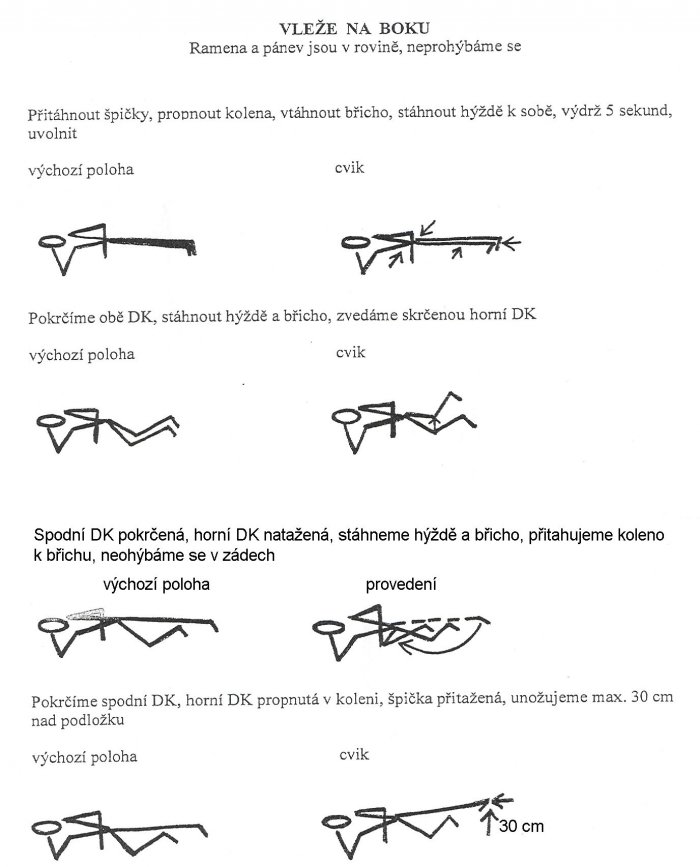

Rehabilitation after cervical spine surgery
Rehabilitation after cervical spine surgery Dear patient, You have undergone cervical spine surgery at the Department of Spondylosurgery, University Hospital in Motol. We would like to provide you with recommendations on how to behave in the home environment after cervical spine surgery. 1. On receipt, you received a fixed Philadelphia neck collar, which is fully paid for by the insurance company. However, the insurance company only pays for the collar per calendar year, so it is very important that you treat the collar with care, as you will have to wear it for six weeks according to your doctor's prescription. The collar should be washed daily with lukewarm water, aggressive detergent should not be used. It is best to wash it with lukewarm soapy water, then rinse with clean water and dry properly. Please do not modify the collar to your liking, as only the standard collar performs its function.
you have completed cervical spine surgery at the Department of Spondylosurgery, University Hospital in Motol. We would like to provide you with recommendations on how to behave in the home environment after cervical spine surgery.
1. Upon receipt, you received a tight Philadelphia neck collar, which is fully paid for by the insurance company. However, the insurance company only pays for the collar per calendar year, so it is very important that you treat the collar with care, as you will have to wear it for six weeks according to your doctor's prescription.
The collar should be washed daily with lukewarm water, aggressive detergent should not be used. It is best to wash it with lukewarm soapy water, then rinse with clean water
and dry properly.
Please do not modify the collar to your liking, as only the standard collar performs its function.
2. The correctly fitted collar must not strangle or be loose. The velcro you fasten it with should be placed on top of each other.
3. When removing the collar, eg during hygiene, avoid rotation of the head and forward bends.
4. You can lie in bed without a collar, with your head from the shoulders underlain by a soft, low-filled pillow. The cervical spine must be level. If you have a restless sleep and are aware of the constant rotation on the bed, you better sleep with your neck collar.
5. The sutures on the neck after anterior access surgery are sewn with absorbable material, so you don't have to come out.
6. The surgical wound on the neck after surgery from the posterior approach is sutured with non-absorbable sutures and therefore must be removed over time. This is usually done (according to the doctor's office) 14 days after the operation.
7. The surgical wound after graft removal is sutured with non-absorbable sutures, so it is necessary to remove them as well. This happens (according to the doctor's office) 14 days after the operation.
8. After 14 days, once the surgical wounds have healed, it is recommended to lubricate them with cream or body lotion to make the scar soft. The scar completely fades
even several months, depending on the ability of the body to regenerate.
Do not soak or bathe surgical wounds. In case of redness, pain, feeling of heat or twitching in the surgical wound, it is necessary to arrange a check-up at the spondylosurgery clinic.
9. Carry out all household chores with the neck collar, loads in the hands may be carried up to a total weight of seven kilograms.
10. Sports is not recommended six weeks after surgery, the only thing that can be recommended is passive exercise. This is an exercise that allows you to maintain full range of motion in the joints and flexibility of muscles and tendons.
11. You do not have to give up sex life, it only depends on you and your partner, or on the choice of a gentle sexual position.
12. You can come to the outpatient clinic of the spondylosurgery department as a co-driver by car or public transport, the ambulance is no longer indicated.
Scar care
The goal of scar care is to heal well and to ensure that the scar moves against the subcutaneous tissue and other structures. It occurs when there are no more scabs on the scar and the skin is completely healed. Let the scar heal, do not tear the scabs around it. Shower the scar for you with a pleasant stream of lukewarm water, but in the first weeks do not soap it, just rinse with water. Keep the scar clean, dry it carefully after bathing and apply a greasy unscented cream to it - this will ensure its suppleness. Apply a so-called pressure massage to the scar (see below). The scar must not be red, hot, purulent and must not bleed.
Pressure massage
Place the thumb of one hand on the lower edge of the scar and lightly press it against the scar with tolerable intensity. After a few seconds, release your thumb, which increases the blood supply to the scar at the site of compression. Follow the same procedure along the entire length of the scar.
Grasp the scar with the so-called fork (between the outstretched index finger and the middle finger) - this will create an eyelash, which you can easily move to the right and left with that "fork". The displacement of the scar is not large at all. Then loosen everything and proceed in the same way along the entire length of the scar.
We wish you a speedy recovery.
The staff of the spondylosurgery clinic
Baggage to the hospital
Bechterew's disease (ankylosing spondylarthritis)
Inflammatory disease of the intervertebral joints causing limited mobility and pain in the spine in adulthood, there is a gradual fusion of the spine to the stage of the so-called bamboo stick
CT (computed tomography)
Based on X-rays, it plays an irreplaceable role in the traumatology of the spine, or in the deformities of the spine, it shows the bone structures of the spine very well.
Discus intervertebralis (intervertebral disc, disc)
Flexible fibrous cartilage plate between two vertebrae of the spine. It absorbs the shocks to which the spine is exposed in everyday life. With increasing age, degenerative changes arise that can lead to herniation
Dorsal Instrumented Spondylo Desis DISD
Surgical procedure in which a certain part of the spine is fixed from the posterior approach using a metal implant.
Dorsal Uninstrumented Spondylosis
Surgical procedure in which a certain part of the spine is fixed from the posterior approach using bone grafts after healing.
Disc herniation (intervertebral disc prolapse)
The intervertebral disc, damaged by degenerative changes, protrudes into the spinal canal (stenosis, narrowing) and can put pressure on the nerve structures, which are manifested, for example, by radiation of pain to the limbs.
Spine instability
Instability is the loss of the ability of the spine to maintain such a position of the vertebrae when exposed to physiological stress that there is no immediate or subsequent injury to the spinal cord and nerve roots and at the same time no developing disabling deformity and severe pain.
Spinal cord
Part of the central nervous system, a string of nerve fibers and cells passing through the spinal canal from the head to about 1-2. lumbar vertebra in an adult, only the nerve roots continue. There are a total of 31 of these roots and they form spinal nerves after exiting the spine.
MRI (magnetic resonance imaging)
Non-invasive examination on the principle of water content in individual tissues, in spinal surgery comes to the fore in determining the condition of the fibrous apparatus, intervertebral discs, spinal cord, refinement and diagnosis of spinal canal narrowing, diagnosis of inflammatory changes and the same degenerative impairment.
Paresis
Partial paralysis (paralysis) of a body part, usually divided into paraparesis - paralysis of the upper or lower limbs from a certain floor and tatraparesis (quadruparesis) paralysis of all limbs, depends on the amount of spinal cord damage, the higher and more damaged, the more severe and extensive the disability body.
Plegia
Complete paralysis of a part of the body caused mostly by complete spinal cord rupture is divided into paraplegia - paralysis of the upper or lower limbs from a certain floor, hemiplegia - paralysis of the right or left half of the body and tetraplegia (quadruplegia) paralysis of all limbs.
PLIF Posterior Interbody Fusion
posterior lumbar intervertebral fusion - a surgical technique in which vertebral body fusion is achieved from the posterior approach using an implant or bone grafts.
A simple x-ray of the spine in two projections
anteroposterior and lateral, basic and indispensable examination of the spine, showing the skeleton of the spine.
Scheurmann's disease
It usually affects adolescents most often aged 12-18 years, more often boys, manifests with increased thoracic curvature of the spine in the anteroposterior sense, pain may occur in 1/5 patients, so-called Schmorl's nodes - herniation of intervertebral discs into vertebral bodies, therapy in most conservative cases - rehabilitation.
Scoliosis
Deformity of the spine in the frontal (frontal) plane - deflection of the spine to the sides. The causes are diverse, such as ulcerative vertebral deformities, unequal limb length, muscle and nerve diseases, and more.
Spondylitis
Inflammatory diseases of the spine joints.
Spondylarthrosis
Degenerative arthritic process affecting the intervertebral joints. It is manifested by back pain, especially after exercise, increased tension in the muscles of the spine, limited mobility.
Spondylitis
Inflammatory diseases of the vertebral body.
Spondylosurgery (spondylosis)
Surgical field dealing with surgical therapy of spinal diseases - injuries, birth defects and deformities, tumors, post-traumatic deformities, degenerative changes.
Spondylodiscitis
Inflammatory disease of the intervertebral disc and adjacent covering plates of the upper and lower vertebrae.
Spondylolisthesis
Displacement (sliding) of the vertebral body of one vertebra forward towards the lower vertebra. According to the size of the shift, it is divided into stages I-IV (according to the% shift). Grade V means a shift by the whole body (more than 100%). This shift is most common in the lower lumbar region, the cause is most often a violation of vertebral development, very rarely as a result of trauma.
Spondylolysis
A condition in which the posterior part of the vertebral arch is interrupted most often due to a congenital disorder of vertebral development, very rarely as a result of an accident. In adulthood, it manifests as instability, which over time can lead to spondylolisthesis.
Spondylosis
Degenerative process affecting the intervertebral spaces. It manifests itself in the reduction of these spaces (intervertebral discs) and the formation of marginal osteophytes at the junction of the vertebral body and disc. Plates (intervertebral discs) lose their elasticity and can become protruding, see disc herniation.
Spondylodesis
Surgical joining (strengthening) of adjacent vertebrae can be instrumented - using a metal implant, or uninstrumented with the help of bone grafts.
Spinal canal stenosis
Narrowing that may be caused by degenerative changes (spondylosis, spondylarthrosis, spondylolisthesis, disc herniation), congenital defects (congenital narrow canal, scoliosis, congenital deformities), injuries, inflammation and tumors of the spine.
PATIENT AFTER HEAD AND LUMBUM
- GETTING UP FROM THE BED
- IN THE OPPOSITE ORDER OF PHOTOS, THE LAYING TO THE BED IS SHOWED
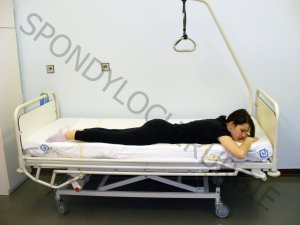
1.
POSITION ON THE ABDOMEN
- the patient turns onto the abdomen
- lies on the edge of the bed
- both upper limbs are at the head
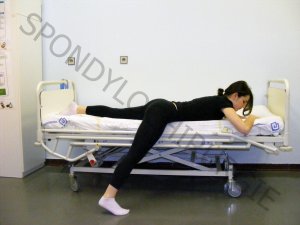
2.a
LOWERING THE LIMBS FROM THE BED TO THE GROUND
- The first lowered limb is the limb closer to the edge of the bed
- the foot touches the ground
- the knee is slightly bent
- the patient's weight begins to be transferred to the lowered lower limb and both elbows
2.b
LOWERING THE LIMBS FROM THE BED TO THE GROUND
- the knee is slightly bent
- The patient's weight is transferred to the lowered lower limb and both elbows, the patient lifts the upper half of the body
- the spine must not be bent at the shoulders!
2.c
LOWERING THE LIMBS FROM THE BED TO THE GROUND
- the patient's weight is constantly transferred to the lowered lower limb
- the weight from the elbows is gradually transferred to both palms
- the spine must not be bent at the shoulders!
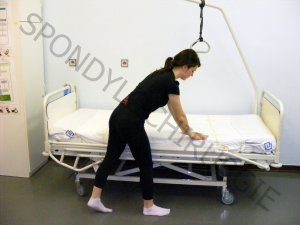
3.
LOWERING THE SECOND LOWER LIMBS ON THE GROUND
- the second lower limb is gradually lowered to the ground
- both knees are slightly bent, the patient is squatting slightly
- the patient's weight is transferred to both lower limbs
- palms lightly touching the bed
- the spine is in one plane
(without excavation of the spine and its rotation)!
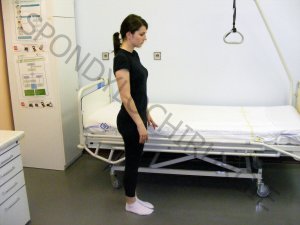
4.
STAND IN THE BED
- straight knees
- flattened spine
- then the patient puts on his crutches
All the steps of getting up and laying in bed follow each other smoothly.
With the promise of the possibility of establishing an independent specialized spondylosurgical department, Dr. In November 2001, Štulík moved from the orthopedic-trauma clinic of the FNKV to the 1st orthopedic clinic of the Motol University Hospital. Here he began to devote himself entirely to spine surgery. Within the standard orthopedic department, three rooms were set aside and one operating day for elective surgery. Traumas were treated separately in the trauma operating room.
Due to the growing number of patients and surgical procedures, it was possible to establish a completely independent department within a few months. On September 1, 2002, the spondylosurgery department of the Motol University Hospital was opened. Organizationally as half of one unit together with the department of neurosurgery for adults, which has been missing in Motol so far. The two separate primates thus had a common secondary medical staff. Operating room for elective operations available on Tuesdays, Thursdays and every even Friday, then gradually every Friday. Subsequently, there was a complete separation of the hall and soon the division of the department, when the neurosurgery moved to the newly allocated premises.
The beginning of the establishment of an independent department dates back to the establishment of the Spondylosurgery Center of the Motol University Hospital, which was established from representatives of individual specializations to determine algorithms for care of patients with spine and spinal cord diseases at the Motol University Hospital and the treatment was rational and as effective as possible.
Since 2007, our workplace has been part of III in terms of teaching. surgical clinics of the 1st Medical Faculty of Charles University and the University Hospital Motol. We are mainly engaged in teaching 5th and 6th year students of the 1st Faculty of Medicine, Charles University and postgraduate education of domestic and foreign doctors in the field of spondylosurgery. We also work closely with the 1st Department of Surgery, 1st Faculty of Medicine, Charles University and General Hospital, 1st Department of Orthopedics, 1st Faculty of Medicine, Charles University and Motol University Hospital, Department of Orthopedics, 1st Faculty of Medicine, Charles University and General Hospital, Department of Orthopedics, XNUMXst Faculty of Medicine, Charles University and Central Hospital.
During its operation, the department ranked first in the classification of domestic workplaces according to the CSCH database of spondylosurgical procedures. The department concentrates up to 25% of all spinal injuries in the Czech Republic, and is also focused on the treatment of primary spinal tumors in children and adults, spinal deformities in children and adults, and craniocervical junction surgery. In the field of extensive tumor resections, the department developed, tested and published new surgical techniques generally accepted in our country and abroad.
Since its establishment in 2002, the Motol Department of Spondylosurgery has published a total of 60 papers in domestic and foreign journals (22 publications in journals with IF, total IF value 29,874, average IF value 1,358). A total of 4 works were awarded the Zahradníček Prize for the best publication of Acta Chir magazine. Orthop. Traumatol. Guild. In 2010, a book was published Cervical spine injuries, which was published in 2012 in the English version as Cervical Spine Trauma. The book won the Chlumský ČSOT Award for the best publication in 2013 and was also awarded by the Rector of Charles University.
On January 1, 2016, the Department of Spondylosurgery of the 1st Medical Faculty of Charles University and the Motol University Hospital was established, as the first of its kind in the Czech Republic, following the example of foreign university centers. This act means a significant contribution to the development of spondylosurgery in the Czech Republic, for its undergraduate and especially postgraduate teaching.
Contact
General contacts
- Secretariat: Zachová Renata, tel .: 224 432 581
Email: renata.zachova@fnmotol.cz - Standard department, tel .: 224 432 573
- ICU, tel .: 224 432 590
- Ambulance, patient ordering, tel .: 224 432 592
- Center for conservative therapy in spondylosurgery, MUDr. Eva Vašková, phone: 224 432 575, 224 432 576
- Admissions office: phone: 224 432 571, fax: 224 432 584
Naděžda Popelková, e-mail: nadezda.popelkova@fnmotol.cz
Václava Masopustová, e-mail: vaclava.masopustova@fnmotol.cz
Tereza Pittnerová, e-mail: tereza.pittnerova@fnmotol.cz
Where to find us?
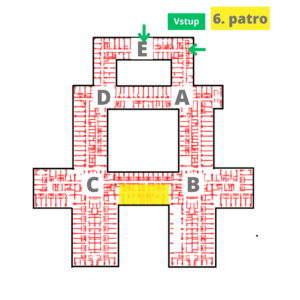 | 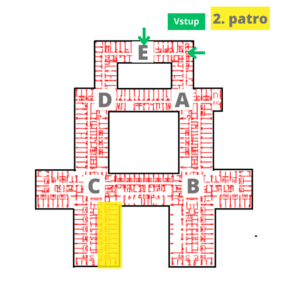 | 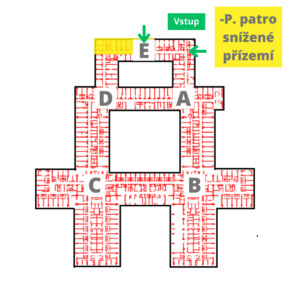 |
|
|
|